Healthcare organizations waste time on fragmented systems where patient information lives in silos and providers can’t communicate efficiently. Patient care coordination tools fix this by connecting everyone involved in a patient’s care-from doctors to insurers to the patients themselves.
We at The Pledge have seen firsthand how the right coordination platform reduces readmissions, cuts costs, and actually improves how patients navigate their own health. This guide walks you through what works and how to implement it.
How Care Coordination Slashes Readmissions and Strengthens Patient Outcomes
Hospitals lose money on readmissions. Medicare penalizes facilities with excess 30-day readmission rates, and unplanned hospital readmissions cost the U.S. healthcare system an estimated $17 billion annually. Care coordination platforms attack this problem directly by ensuring patients don’t fall through cracks between discharge and home recovery. When providers use integrated coordination tools, they track patient status in real time, catch complications before they escalate, and send timely reminders for follow-up appointments and medication adherence. Research from the VA system, which operates one of the most coordinated care networks in America, found that warm handoffs between primary care and specialists enabled by shared digital platforms strengthen relationships between clinicians and accelerate patient access to services. The same principle applies in commercial healthcare: when your care team communicates through a centralized system instead of phone tag and faxes, patients recover faster and avoid preventable ER visits.
What Real Coordination Looks Like in Practice
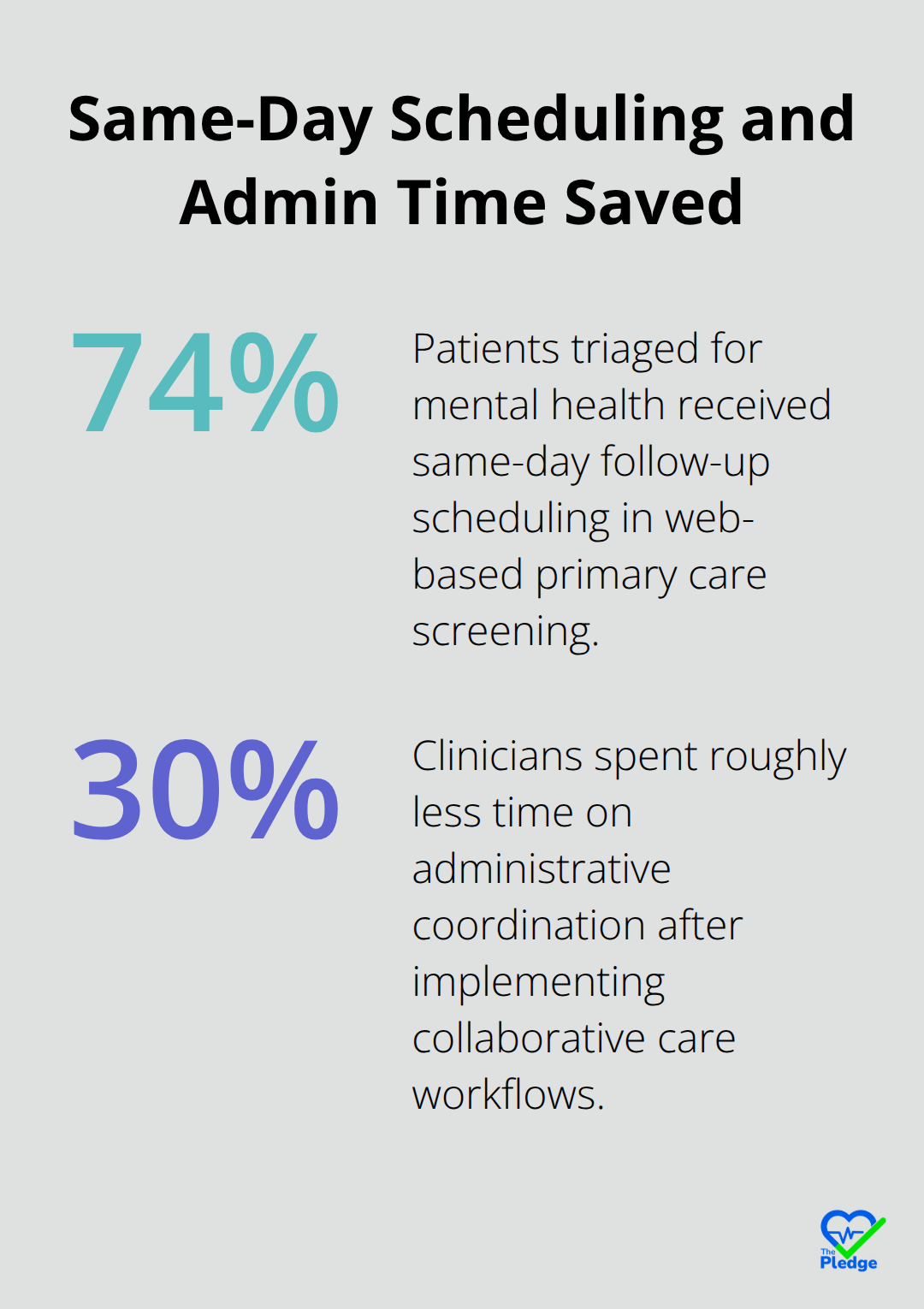
Physical proximity matters far less than digital proximity. The VA study of 102 clinicians across eight sites revealed that sites with strong care coordination reported consistent use of shared digital tools and clear communication protocols, while low-performing sites struggled with fragmented systems and staffing turnover. This tells you something critical: the platform itself is only half the battle. Staffing stability and cross-disciplinary relationships drive the other half. When your organization implements a care coordination tool, prioritize adoption training and give your team time to build workflows around it. Automated appointment reminders alone reduce no-shows by significant margins; one study of web-based screening in primary care found that 74% of patients triaged for mental health concerns received scheduling for follow-up the same day. Proactive outreach works.
The moment a patient’s lab results come back abnormal or a discharge summary indicates a high-risk condition, your coordination platform should flag it and assign it to the right team member. This isn’t about sending more messages-it’s about sending the right message to the right person at the right time.
Connecting Prevention to Cost Reduction
Prevention doesn’t happen by accident. Coordinated care platforms embed preventative workflows into daily operations through automated task sequencing and flagging of patients due for screenings or vaccinations. When providers see these reminders integrated into their workflow instead of buried in a separate system, they act on them. The IMPACT collaborative care model for managing late-life depression showed that coordinated care reduced depression severity and increased treatment engagement, with an annual cost per patient of roughly $533-far cheaper than treating a preventable crisis. The key is that coordination tools give clinicians visibility into what’s already been done and what’s next, eliminating duplicate tests and unnecessary specialist visits. If your organization manages patients with chronic conditions across multiple departments, a centralized platform showing medication history, recent test results, and current care stage prevents costly redundancy and keeps patients engaged in their own recovery.
Building the Foundation for Sustainable Coordination
Staffing stability and cross-disciplinary relationships form the backbone of effective care coordination. Sites that maintained consistent teams reported stronger coordination outcomes than those with high turnover. Clear service agreements between departments also matter; high-performing sites clarified which conditions trigger referrals and which team owns each handoff, eliminating confusion and delays. When your organization selects a coordination platform, test it with a pilot group first. Train staff thoroughly on how to use shared digital tools, and measure adoption rates weekly. The platform succeeds only when clinicians actually use it, so remove barriers to adoption and celebrate early wins. Strong professional relationships between primary care, mental health, and specialty care teams accelerate information flow and improve patient outcomes. These relationships deepen when teams work side by side-whether physically or through frequent digital collaboration-and when leadership removes silos that pit departments against each other.
What Modern Coordination Platforms Actually Do
Modern care coordination platforms eliminate the manual work that slows down patient navigation. Instead of clinicians piecing together information from multiple systems, a centralized platform displays each patient’s complete health picture in one place. Lab results, medication lists, insurance coverage details, and appointment history sit side by side. When a patient’s test results change, the system flags the relevant providers automatically and assigns follow-up tasks to the right team member.

Real-time data access cuts the time clinicians spend hunting for information; providers spend less time on administrative tasks and more time on patient care when data consolidates into one view. The most effective platforms embed themselves directly into the workflows clinicians already use daily, not as a separate tool that requires context switching. This integration matters because adoption fails when staff must toggle between systems.
Automated Reminders and Real-Time Task Assignment
Automated appointment reminders address one of the biggest coordination failures: no-shows and missed follow-ups. Mobile text message reminders improved rate of attendance compared to no reminders. This speed prevents patients from falling out of the care pathway. The platform should also surface insurance benefits and cost transparency without forcing patients to guess what their coverage includes. When patients see out-of-pocket costs upfront, they engage more honestly with their care team about treatment options. Organizations that implement these platforms see measurable drops in duplicate testing, fewer authorization delays, and better medication adherence because reminders reach patients at the right moment in their care journey.
Staffing Capacity and Platform Adoption
Staffing capacity and platform usability determine whether coordination tools actually improve outcomes or sit unused. High-performing organizations assign someone to monitor adoption rates weekly and remove barriers when clinicians struggle with the interface. The VA research showed that sites with dedicated staff supporting the coordination platform sustained better outcomes than sites that deployed the tool and expected clinicians to figure it out independently. Integration with existing systems matters tremendously; platforms that require manual data entry or don’t connect with your current EHR will face resistance. Cost transparency features should pull real-time data from insurance systems rather than displaying generic estimates. When a patient books an imaging test, they should see the actual negotiated rate at that facility within seconds. This transparency builds trust and prevents bill shock, which drives patient engagement.
Testing and Measuring What Actually Works
Organizations should test the platform with a single department or pilot group before organization-wide rollout. Measure which features clinicians actually use and which ones they ignore, then adjust training accordingly. The goal is not adoption for adoption’s sake but rather adoption that translates to fewer readmissions, shorter time to treatment, and patients who stay engaged in their own care. Once you identify which features drive real clinical value, you can scale confidently across your organization and prepare your teams for the operational changes that come next.
How to Roll Out Care Coordination Without Disrupting Operations
Successful care coordination deployment requires a different approach than standard software installation. You’re not just changing tools; you’re transforming how clinicians work and how information flows through your organization. Start by mapping your current state honestly. Where do your teams spend the most time on administrative tasks versus patient care? The VA research across eight sites found that high-performing organizations identified specific bottlenecks before selecting a platform, then chose solutions that addressed those exact pain points rather than adopting the most feature-rich option available.

Identify Your Bottlenecks First
Interview your frontline staff-nurses, schedulers, clinicians, and billing staff-about what slows them down daily. You’ll likely hear about switching between systems, duplicate data entry, missed follow-up opportunities, and poor visibility into what other departments are doing. These aren’t minor complaints; they’re your roadmap. One organization that implemented collaborative care for depression found that clinicians spent roughly 30 percent less time on administrative coordination when the platform eliminated manual handoff processes. Document these inefficiencies with specifics: How many minutes per day does your scheduler spend on phone tag with specialist offices? How many tests get repeated because results don’t reach the ordering provider? These numbers justify the investment and set a baseline for measuring success after implementation.
Prioritize Integration Depth Over Feature Count
Your platform selection matters far less than integration depth and staff adoption. Most care coordination tools fail not because they lack features but because clinicians resist using them. The platform must launch directly inside your existing EHR or workflow system, not as a separate tab that requires context switching. If your team uses Epic, the coordination tool should appear as an app within Epic’s interface. If you rely on another EHR, confirm the vendor offers deep integration before signing the contract. Platforms that require manual data entry or don’t connect with your current systems will face resistance from day one.
Test With a Pilot Group Before Full Rollout
Test the platform with a single department or clinic for 8–12 weeks before rolling out organization-wide. Choose your pilot group strategically; select clinicians who are neither technology-averse nor early adopters, but rather representative of your typical staff. Measure adoption weekly by tracking login frequency, task completion rates, and which features get used versus ignored. Most organizations see adoption rates of 40–60 percent in the first month, climbing to 70–85 percent by month three if training is thorough and barriers are removed quickly.
Assign one staff member to monitor adoption metrics and troubleshoot issues in real time; this role prevents the platform from sitting idle while clinicians continue old workflows. When clinicians struggle with a feature, don’t assume they’re resisting change-assume the feature is unclear or doesn’t fit their workflow. Adjust training or reconfigure the tool accordingly. The goal is adoption that translates to measurable outcomes: fewer readmissions, shorter time to treatment, and reduced administrative burden, not adoption for its own sake.
Remove Barriers to Adoption Immediately
Staffing capacity and platform usability determine whether coordination tools actually improve outcomes or sit unused. High-performing organizations assign someone to monitor adoption rates weekly and remove barriers when clinicians struggle with the interface. The VA research showed that sites with dedicated staff supporting the coordination platform sustained better outcomes than sites that deployed the tool and expected clinicians to figure it out independently. Cost transparency features should pull real-time data from insurance systems, including related care before and after the primary procedure such as office visits and imaging procedures. When a patient books an imaging test, they should see the actual negotiated rate at that facility within seconds. This transparency builds trust and prevents bill shock, which drives patient engagement.
Final Thoughts
Care coordination tools work because they address a fundamental problem: healthcare organizations operate in silos, and patients pay the price. When you implement patient care coordination tools that integrate your systems, automate handoffs, and give clinicians real-time visibility into patient status, readmissions drop, costs fall, and patients engage in their own recovery. The VA research across eight sites proved this repeatedly-organizations with strong coordination reported fewer preventable complications, faster access to specialists, and clinicians who spent less time on administrative work and more time on care.
The long-term impact compounds over time. A hospital that reduces 30-day readmissions by even 5 percent avoids millions in Medicare penalties annually. An employer that implements coordination tools sees employees miss fewer workdays and engage more actively in preventative care, which cuts downstream costs significantly. Patients who receive timely appointment reminders and have transparent visibility into their care plan stay adherent to treatment and avoid costly emergency visits.
Your next step depends on your role. If you lead a healthcare organization, audit your current workflows honestly, identify your biggest bottlenecks, and select a platform that integrates deeply with your existing systems rather than adding another tool to your stack. The Pledge centralizes health data, sends personalized reminders, and integrates seamlessly with existing health plans-giving employees and employers the visibility and automation needed to transform care navigation. Start with a pilot, measure what works, and scale confidently.