Your employees are drowning in healthcare complexity. Medical records live in different systems, specialists don’t talk to each other, and your workforce wastes time piecing together their own care.
At The Pledge, we’ve seen this problem destroy both employee wellbeing and your bottom line. A care navigation overview shows you how to fix it-by centralizing health information, coordinating care across providers, and giving your team actual control over their health.
Why Your Healthcare System Is Costing You More Than It Should
The Fragmentation Problem
Your employees navigate a healthcare system designed for fragmentation. Medical records sit in hospital systems, pharmacy data lives in separate software, and insurance information resides in yet another portal. 65% of Americans say coordinating and managing healthcare is overwhelming and time-consuming. This isn’t just an inconvenience-it costs you money. According to research from the U.S. Office of Disease Prevention and Health Promotion, 94.7% of adults don’t receive all recommended preventive care, largely because they can’t figure out what they need or where to get it. When employees skip preventive care, they develop expensive complications later.
The CDC defines healthcare literacy as the ability to find, understand, and use information and services to inform health-related decisions, and most of your workforce lacks it. Without a centralized system, employees make healthcare decisions based on emotion and convenience rather than value, often selecting the most expensive option simply because it’s familiar or closest to their office.
The True Cost of Wasteful Spending
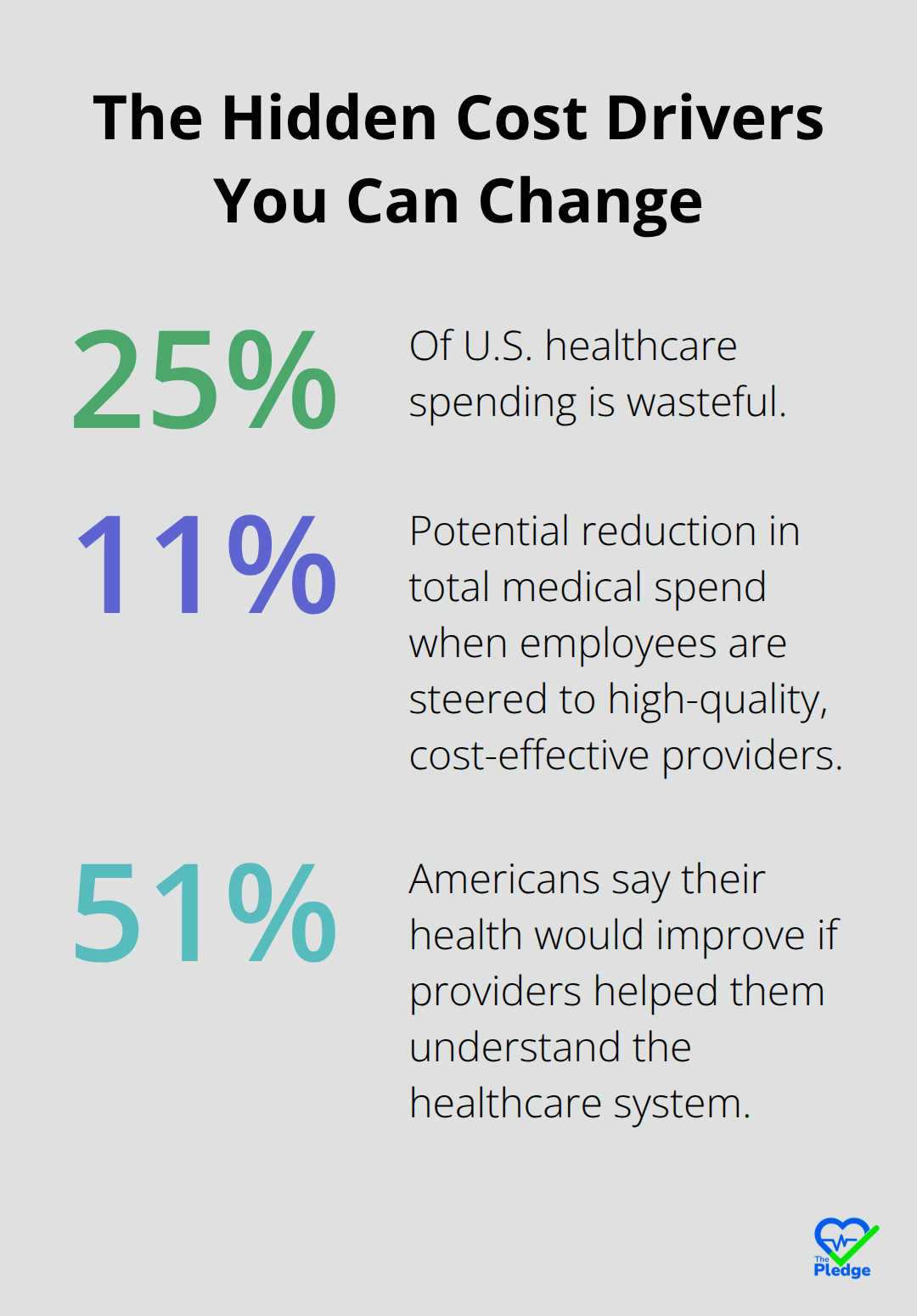
The cost impact is staggering. 25% of U.S. healthcare spending is wasteful. With the nation spending $4.9 trillion on healthcare in 2023, that means roughly $1.2 trillion went toward unnecessary care, duplicative services, and preventable complications. For your organization, this translates to about $3,687 per employee per year in avoidable spending.
A single procedure costs five to ten times more across different facilities, driven entirely by care setting rather than quality differences. Your employees don’t know this variation exists, so they default to whoever their doctor mentions or whoever their insurance card directs them to. Without visibility into where your employees seek care and why they choose expensive options, you operate without critical information on your healthcare spend.
Why Reactive Approaches Fail
Most employers lack real-time insight into utilization patterns until claims arrive weeks later, making intervention impossible. This reactive approach leaves your organization absorbing the costs of fragmented care, preventable readmissions, and unnecessary specialist visits that coordination could have prevented. Your benefits team reacts to problems instead of stopping them before they start.
The gap between what you spend and what you actually need to spend represents a massive opportunity. Closing this gap requires visibility into employee health decisions at the moment they happen, not after the bills arrive. This is where care navigation transforms your approach from reactive cost management to proactive health orchestration.
What Care Navigation Actually Does for Your Workforce
Beyond the Portal: Active Orchestration
Care navigation isn’t a portal. It’s not another login screen buried between your benefits site and a pharmacy app. Care navigation represents active orchestration-a system that brings together medical records, pharmacy data, insurance eligibility, and provider networks into one functional workspace where employees make decisions with complete information. The difference between passive care navigation and active orchestration matters significantly. Passive systems show employees a list of providers and their costs. Active systems tell employees which provider is in-network, what they’ll pay out-of-pocket for a specific procedure, whether that provider has good outcomes for their condition, and then books the appointment. According to Healthcare Bluebook’s decade of data, employers who steer employees toward high-quality, cost-effective providers see up to 11% reduction in total medical spend. That’s not theoretical-that’s what happens when your workforce stops defaulting to expensive options and starts making informed choices.
How Real Coordination Eliminates Fragmentation
Real coordination eliminates the cascade of problems that fragmented systems create. When a specialist receives records from a primary care physician through an integrated navigation system, they don’t repeat tests or prescribe conflicting medications. When pharmacy data flows into the same system as medical records, navigators catch drug interactions before they become hospitalizations. When benefits data updates in real-time, employees know immediately whether a new treatment option is covered or requires prior authorization-they don’t find out after scheduling surgery. This integration transforms how care actually happens across your organization.
Proactive Health Interventions: Where Real Savings Happen
The proactive layer matters most. Harris Poll research shows 51% of Americans say their health would improve if providers helped them understand the healthcare system. Proactive health interventions powered by AI don’t wait for employees to ask questions. They monitor health data, recognize when someone needs preventive screening, identify at-risk conditions before complications develop, and send timely reminders with actionable next steps. An employee with pre-diabetes receives a message about available nutrition programs and glucose monitoring support before they need insulin therapy. A member with a new medication that has available copay assistance programs gets notified immediately, not months later when they’ve already paid full price. This shift from reactive to proactive is where cost reduction actually happens-preventing expensive problems costs far less than treating them.
The real power emerges when navigation systems connect this proactive intelligence to your benefits design. Your team gains visibility into which employees engage with preventive care, which ones need additional support, and where your health plan design either encourages or discourages healthy behaviors. This visibility transforms how you build your benefits strategy moving forward.
How to Build Your Care Navigation Implementation
Audit Your Data Landscape First
Implementing care navigation requires moving beyond vendor selection to architectural design. Your organization must decide whether you’re bolting navigation onto your existing benefits infrastructure or rebuilding how benefits actually function. We at The Pledge believe the second approach delivers measurable results. The difference matters because navigation systems only work when they sit at the center of your benefits strategy, not at the periphery.
Start with a complete audit of your current data landscape. Where do your health plan records live? What systems hold pharmacy data? Which platform manages your eligibility information? Most organizations discover their data lives in three to five disconnected systems, making real-time coordination impossible. A unified care navigation platform consolidates this data into a single source of truth, enabling navigators and AI systems to make decisions with complete information.
This consolidation step is where 37% of employers currently stop, according to Employee Benefit News survey data. They implement navigation tools but fail to fully integrate underlying data systems, leaving their workforce still jumping between portals. Demand that your navigation vendor connects directly to your claims data, eligibility systems, and pharmacy records. The integration should be bidirectional, meaning when benefits change, the navigation system updates immediately.
Identify At-Risk Employees With AI-Driven Analysis
AI-driven identification of at-risk employees separates effective programs from expensive ones that feel good but miss the people who need help most. Your navigation system should analyze claims patterns, lab results, medication fills, and engagement signals to surface employees likely to develop costly complications. An employee filling diabetes medications but never attending preventive visits needs outreach. Someone with a new cancer diagnosis needs coordinated care scheduling and financial counseling before treatment begins. A member approaching their deductible needs to understand what preventive services are now free.
These interventions only work when they reach people at the moment they matter most, not months after claims arrive. Your navigation vendor should provide real-time reporting showing which employees your system identified as at-risk, what interventions were offered, and whether they engaged. This visibility transforms how you build your benefits strategy moving forward.
Enable Family Participation in Care Decisions
Family participation transforms individual health management into coordinated household health. The Pledge includes Family Share functionality, allowing employees to include spouses, adult children, and aging parents in their care decisions. A daughter managing her mother’s medication adherence can receive appointment reminders. A spouse can access cost information when making decisions about joint procedures. This family-centered approach reflects how healthcare actually happens in most households, not the individual-focused model most benefits assume.
When you implement care navigation, explicitly design for multi-person households and give employees control over what information family members can access. This shift recognizes that healthcare decisions rarely happen in isolation-they involve conversations with loved ones, shared financial responsibility, and coordinated schedules across multiple people.
Final Thoughts
Care navigation transforms how your organization manages employee health and eliminates the waste that fragments your workforce’s healthcare experience. Employers who steer employees toward high-quality, cost-effective providers see up to 11% reductions in total medical spend, and this care navigation overview shows you exactly how to achieve those results. Your employees gain control over their health journey, knowing exactly what procedures cost, which providers deliver better outcomes, and what support programs are available to them.
Strategic implementation requires commitment beyond vendor selection-you must audit your data landscape, integrate systems into a single source of truth, and position care navigation at the center of your benefits strategy. When you complete this work, your organization gains real-time visibility into how employees access care, which interventions drive engagement, and where your benefits design either supports or undermines healthy behaviors. Long-term workforce wellness emerges from this foundation, as employees who understand their healthcare options and receive proactive support for managing chronic conditions stay healthier and more productive.
Start your implementation by auditing your current data landscape and identifying which systems hold your health information. Then connect with a navigation vendor committed to full integration rather than surface-level tools. Explore how The Pledge can centralize your employee health management and transform your benefits strategy into a proactive health orchestration system.










