Surgical scheduling coordination failures cost hospitals millions annually while putting patients at risk. Operating room delays cascade through entire healthcare systems, wasting resources and compromising care quality.
At The Pledge, we’ve seen firsthand how the right technology transforms scheduling chaos into seamless coordination. This guide shows you exactly how care navigation solutions eliminate delays and improve outcomes.
What Surgical Delays Actually Cost Your Hospital
Operating rooms generate over 40% of hospital revenue and consume roughly 30% of total hospital expenditures, according to research by Amin, Baldacci, and Kayvanfar. This makes surgical scheduling not just a logistical issue but a direct financial lever. When delays happen, hospitals hemorrhage money fast. A study across five Iranian teaching hospitals found that interruptions and delays consumed 7,920 minutes of surgical time across 251 surgeries, averaging 30 minutes of lost time per case. That’s 16.83% of total operating room time vanishing to preventable disruptions. With annual US operating room costs estimated at 30 to 90 billion dollars, even modest improvements in scheduling precision translate into millions in recovered revenue.
Where the Money Disappears
The culprits behind delays reveal themselves clearly when you track them. Operating room staff caused 53.91% of interruptions and delays, with late arrivals of surgical attendings and anesthesia teams accounting for 27 and 20 events respectively. Equipment and instrument problems contributed another 18.80% of disruptions, including insufficient devices and broken equipment that force rescheduling.

Bed availability constraints and ICU bottlenecks created additional cascades, blocking downstream admissions and compressing the surgical schedule. Managerial issues like poor planning and shift-change conflicts added another 10.34% of delays. When you add patient-related factors like unstable vitals or incomplete pre-operative clearances, the picture becomes clear: surgical delays stem from fragmented communication and incomplete pre-operative readiness. Each preventable delay represents direct cost loss plus indirect expenses from staff overtime, equipment idle time, and reduced throughput.
The Patient Safety Equation
Delays don’t just cost money; they compromise patient safety. Extended anesthesia exposure increases infection risk and post-operative complications. When surgeries run late, recovery beds fill unpredictably, forcing rushed discharge planning or ICU overflow. Research shows that approximately 71.32% of surgeries experience at least one interruption or delay, meaning most patients face some level of schedule disruption. Incomplete pre-operative clearances, missing insurance authorizations, and miscommunication between departments force last-minute cancellations that destabilize patient care plans. A hospital in Egypt improved booking compliance from 64.7% to 89.7% within three months simply through electronic surgical booking, simultaneously increasing elective surgical volume by 31% while saving 63 operating room hours monthly. That same hospital prevented roughly 126 improperly scheduled cases per month and saved approximately 126,000 EGP in direct costs.

The data is unambiguous: better scheduling coordination directly improves patient outcomes while protecting revenue.
Why Coordination Matters Now
These numbers expose a critical truth: hospitals that fail to coordinate surgical scheduling lose both money and patient trust. The gap between current performance and what’s possible widens every month. A 25-percentage-point improvement in booking compliance (as the Egyptian hospital achieved) doesn’t happen through incremental tweaks-it requires systematic change. The next section reveals how care navigation solutions close this gap and what specific capabilities transform scheduling from a chronic pain point into a competitive advantage.
How Care Navigation Solutions Close Scheduling Gaps
Care navigation platforms eliminate the information silos that create surgical delays. Instead of coordination happening across disconnected email threads, phone calls, and paper charts, these systems create a single source of truth where every stakeholder sees real-time status updates.
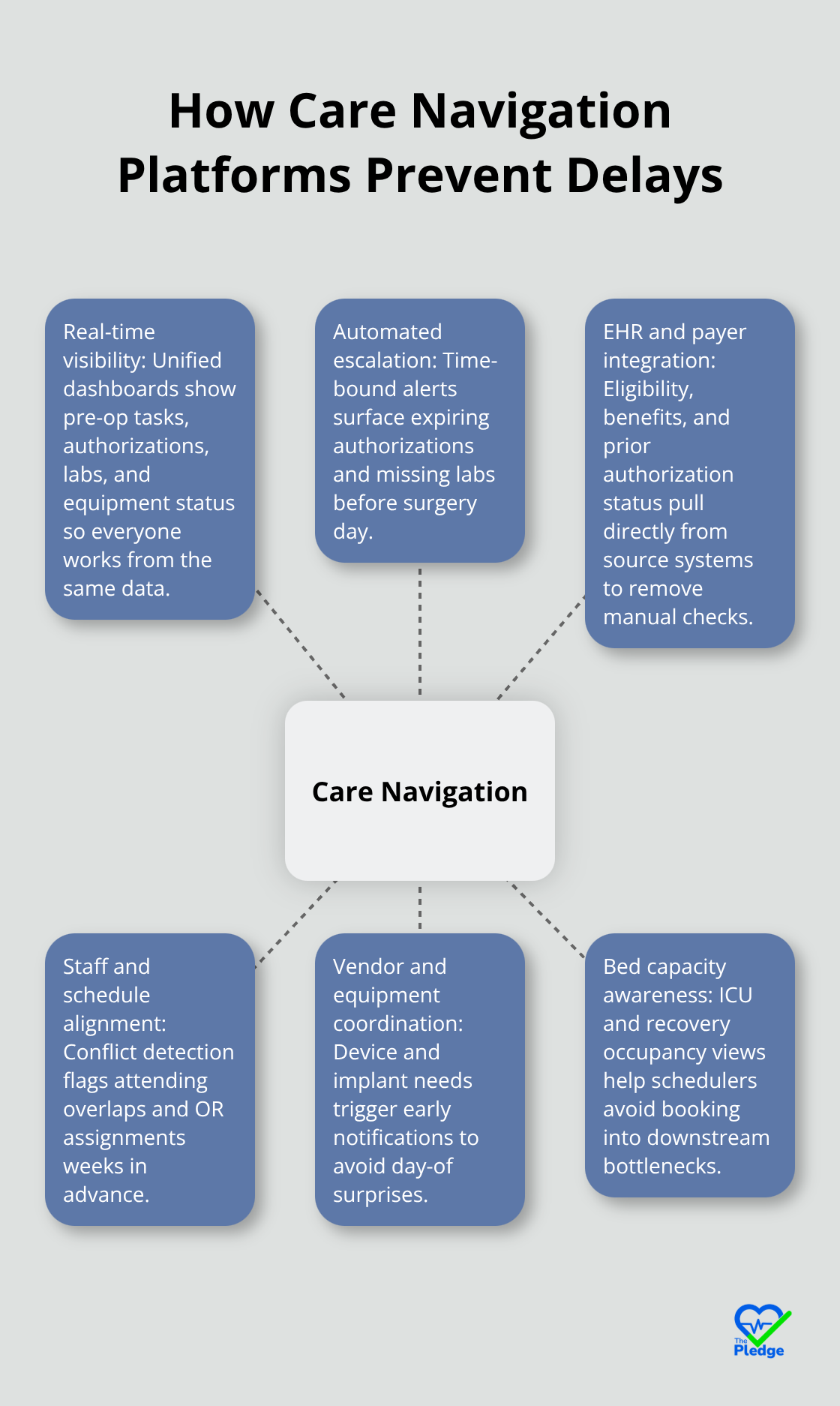
A hospital in Egypt implemented electronic surgical booking and watched booking compliance jump from 64.7% to 89.7% within three months. That improvement came directly from centralized visibility: when insurance teams, surgical schedulers, and pre-operative coordinators access the same system simultaneously, expired authorizations get caught before surgery day arrives. The platform automatically flags when a CPT code lacks prior authorization or when a patient’s lab work hasn’t been completed, preventing the cascade of last-minute cancellations that consumed 16.83% of operating room time in teaching hospital research. Real-time coordination also catches equipment and vendor delays upfront. If a specific implant requires a device representative present, the system notifies the vendor weeks in advance rather than discovering the gap on surgery morning.
Automating Pre-Operative Details That Derail Surgery
Manual pre-operative processes fail because they rely on human memory and scattered communication channels. Care navigation platforms eliminate this vulnerability through automated reminders targeted at patients, providers, and support staff. A patient receives specific pre-operative instructions via the app-nothing vague about fasting, but exact times and dietary restrictions mapped to their surgery start time. Surgical staff receives alerts about missing clearances or outstanding lab results, with direct links to order or review them. Insurance coordinators get notifications when surgery dates shift, triggering immediate reauthorization checks before the original approval expires. Integration with provider and insurance data means the system pulls eligibility information, benefit details, and prior authorization status directly from source systems rather than relying on staff to manually verify each element. When a patient’s insurance changes or coverage lapses, the platform flags it immediately instead of discovering the problem during pre-operative verification.
Connecting Departments Through Structured Handoffs
Surgical delays stem largely from departments operating independently. Care navigation solutions create structured handoff protocols where information flows predictably between pre-operative holding, the operating room, recovery, and post-operative units. Rather than assuming the surgical team knows about a patient’s previous adverse reaction to anesthesia or special positioning needs, the system surfaces this information automatically at each transition point. When the system displays a surgeon’s schedule and operating room assignments in one view, conflicts become visible weeks ahead instead of minutes before start time. This approach directly supports improved coordination across surgical teams-more cases fit the schedule because coordination problems are solved before they create bottlenecks.
Moving From Reactive to Proactive Scheduling
The shift from manual to electronic surgical booking transforms how hospitals respond to scheduling challenges. Instead of reacting to problems on surgery day, care navigation platforms enable teams to identify and resolve conflicts during the planning phase. Hospitals that adopt these systems report measurable improvements across multiple specialties: obstetrics and gynecology booking compliance rose from 39.1% to 75.0%, vascular surgery improved from 56.9% to 94.9%, and maxillofacial surgery increased from 54.5% to 84.4%. These gains reflect a fundamental change in how surgical teams operate-they work from complete, current information rather than incomplete data scattered across departments. The system’s real-time availability checks and automated conflict resolution mean that scheduling staff spend less time troubleshooting problems and more time optimizing the surgical calendar. This efficiency gain directly translates to higher utilization rates and more predictable operating room performance. The next section reveals what specific capabilities separate effective care navigation platforms from basic scheduling tools, and how to evaluate solutions that will actually transform your surgical operations.
Building a Care Navigation Platform Into Your Surgical Operations
Selecting Platforms That Prevent Your Specific Delays
Selecting the right care navigation platform requires understanding what actually moves the needle in surgical coordination. Focus on platforms that deliver three core capabilities: real-time visibility across all pre-operative tasks, automated escalation when deadlines approach, and direct integration with your existing hospital information systems. The platform must surface which cases lack prior authorization, which patients haven’t completed required lab work, and which surgeries face equipment delays-all in a single dashboard that your scheduling team checks daily. Platforms that simply digitize paper forms miss the point entirely. What matters is whether the system prevents the specific delays your hospital experiences. If your teaching hospital loses 53.91% of surgical time to staff-related delays like late arrivals of surgical attendings, the platform must alert scheduling coordinators when an attending’s schedule conflicts with assigned cases, weeks before surgery day. If bed availability creates bottlenecks, the system should show real-time ICU and recovery bed occupancy so schedulers avoid booking cases when downstream capacity doesn’t exist.
Integration with your EHR and insurance verification systems eliminates manual data entry that introduces errors and consumes coordinator time. The platform should automatically pull insurance eligibility, benefit details, and prior authorization status directly from payers rather than requiring staff to telephone for verification. When a patient’s coverage changes, the system should flag it immediately during pre-operative review rather than discovering the problem on surgery morning.
Redesigning Workflows Around Technology, Not Fitting Technology Into Workflows
Implementation succeeds when you treat the transition as a department-wide process redesign, not a software installation. Start by mapping your current pre-operative workflow across all stakeholders-surgical schedulers, insurance coordinators, pre-operative nurses, operating room staff, and recovery unit managers. Document where information gets lost, where departments duplicate effort, and where deadlines slip. One hospital improved booking compliance improvements surgical specialties by redesigning their entire pre-operative process around the electronic system rather than simply uploading existing workflows into software. Staff training and change management proved critical to their success. Your team needs to understand not just how to use the platform, but why each automated step matters. A scheduling coordinator who understands that automated prior authorization checks prevent improperly scheduled cases will adopt the system enthusiastically.
Piloting Before Hospital-Wide Rollout
Start with one surgical specialty-perhaps the one with your highest cancellation rate-and run pilot operations for two to three months before hospital-wide rollout. This approach lets you refine workflows and train staff without disrupting your entire surgical calendar. The pilot phase reveals which automated alerts actually prevent delays and which ones create noise that coordinators ignore. You’ll discover whether your insurance verification process needs adjustment or whether your pre-operative nursing protocols require modification to work with the new system. Staff who participate in the pilot become champions during broader implementation because they’ve experienced the benefits firsthand.
Measuring Performance That Matters
Measure performance through metrics that matter: first-case on-time starts, same-day cancellation rates broken down by cause, prior authorization compliance, and operating room utilization rates. Try to approach the 75–85% utilization range that high-performing practices target. Most importantly, measure whether booking compliance improves across your surgical specialties. These improvements happen within three months when implementation combines technology with trained human operators who understand surgical coordination requirements.
Final Thoughts
Surgical scheduling coordination transforms from a chronic operational headache into a competitive advantage when hospitals implement care navigation solutions. The data proves this unambiguously: hospitals that centralize scheduling information, automate pre-operative verification, and integrate insurance data see booking compliance jump by 25 percentage points within months while simultaneously increasing surgical volume and reducing costs. These improvements represent fundamental shifts in how hospitals operate, not marginal gains that fade over time.
Operating rooms generate over 40% of hospital revenue, making scheduling precision a financial lever that moves the entire organization. The 63 operating room hours saved monthly by one hospital, multiplied across your facility’s surgical calendar, translates into millions in recovered revenue annually. More importantly, that recovered capacity means more patients receive timely surgical care rather than waiting on cancellation lists, while staff work from complete information instead of fragmented data that introduces errors and frustration.
Moving forward requires treating surgical scheduling as a strategic priority, not an administrative task. The hospitals achieving the highest performance metrics-75 to 85% utilization rates, minimal same-day cancellations, strong first-case on-time starts-share one characteristic: they invested in technology combined with trained coordinators who understand surgical workflow requirements. The Pledge provides exactly this combination, centralizing surgical scheduling data while enabling real-time coordination across all stakeholders.










