Healthcare costs keep climbing for employers. In 2025, companies are spending more on prescription drugs, emergency room visits, and managing chronic diseases than ever before.
We at The Pledge know that reducing healthcare costs doesn’t mean cutting corners on employee health. It means using smarter strategies-from preventative care to digital health platforms-that actually work.
What’s Driving Healthcare Costs Up for Your Company
Prescription Drug Spending Spirals Out of Control
Prescription drug spending dominates your healthcare budget. According to the Business Group on Health, pharmacy now accounts for 27% of total healthcare spending in 2024, up from 21% in 2021. This shift matters because your pharmacy bill grows faster than your medical bill. GLP-1 medications for diabetes and weight management cost around $700 to $800 per month per person. An estimated 57.4 million privately insured adults under 65 are eligible for these drugs, and utilization keeps climbing.

U.S. drug prices run 4.22 times higher than in other developed countries, a gap driven by patents and pricing practices that keep branded medications expensive.
Wellness programs and generic substitution campaigns alone won’t solve this problem. You need a pharmacy strategy that decouples coverage from rebates, considers biosimilar adoption, and implements stricter coverage criteria for high-cost therapies.
Emergency Department Overuse Drains Your Budget
Emergency department overuse represents another major drain on your budget, though it’s often preventable. Many employees treat the ER as urgent care, driving unnecessary claims for conditions that primary care or telehealth could manage. Quantum Health data shows that telehealth and urgent care expansion reduce ER visits and save about $15.65 per member-month. The real issue is access to primary care. When employees can’t get timely appointments with their primary care doctor, they default to the ER.
Chronic Disease Management Gaps Compound Costs
Chronic disease management gaps compound this problem significantly. According to data from the Business Group on Health, rising rates of cancer, cardiovascular disease, diabetes, and mental health conditions drive escalating costs, especially when early intervention is missed. The Commonwealth Fund emphasizes that value-based care models reduce overall costs by emphasizing primary care and cutting unnecessary ER and hospital use.
Musculoskeletal care alone represents one of the largest cost drivers in many employer plans, yet much of it is avoidable through early, conservative treatment rather than imaging and surgery. Your job is to identify which conditions cost you the most, then steer employees toward high-quality providers and care pathways that catch problems early. This targeted approach sets the stage for implementing the preventative care programs and digital tools that actually move the needle on costs.
What Actually Works to Lower Healthcare Spending
Design Preventative Care Around Your Real Cost Drivers
Preventative care programs work, but only when you build them around the conditions that actually drain your budget rather than generic wellness activities. The Commonwealth Fund research shows that value-based care models reduce overall costs by emphasizing primary care and cutting unnecessary ER and hospital use. However, 88% of employers rate health-related benefits as very important while only 39% offer structured wellness programs with real resources behind them. This gap exists because most wellness initiatives lack teeth.
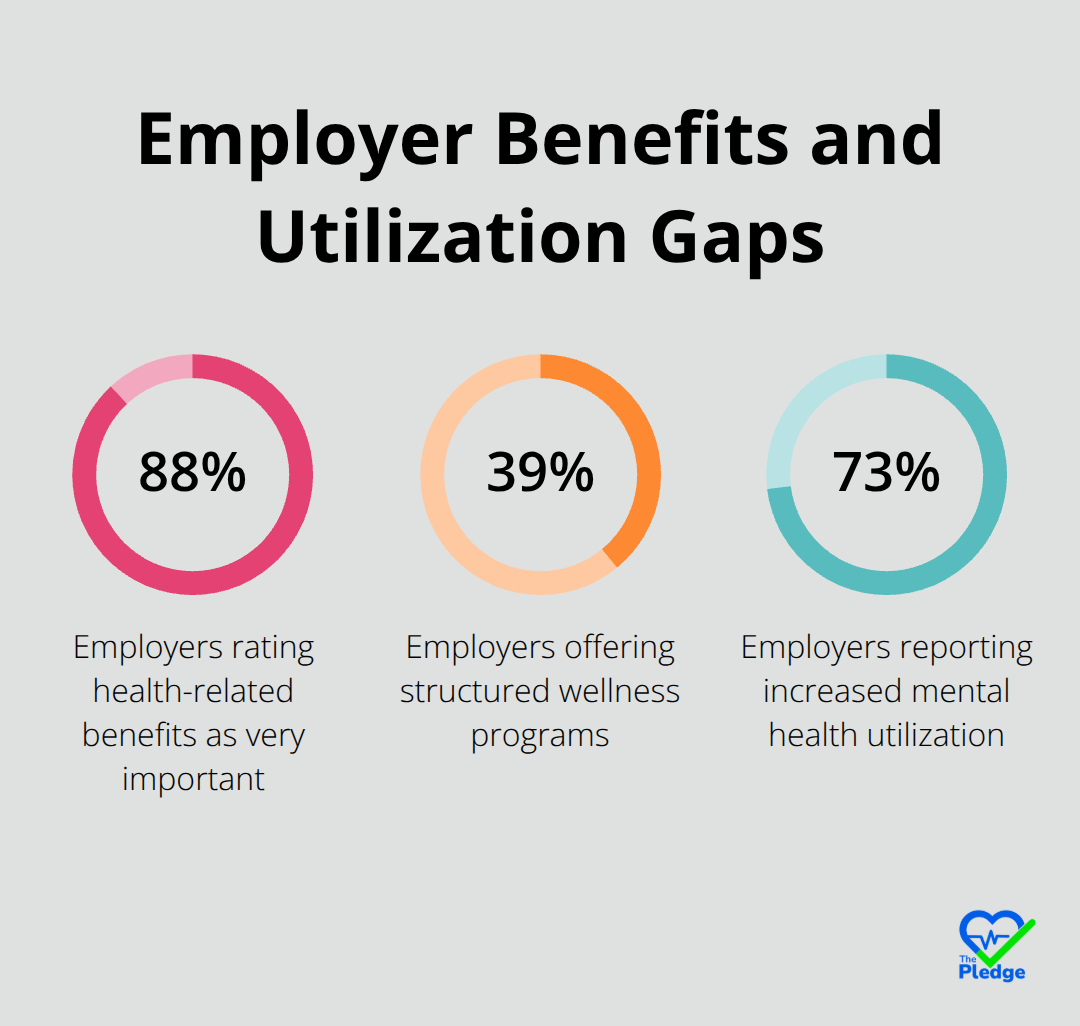
Your program needs to target the conditions that consume your budget. Cancer, cardiovascular disease, diabetes, and mental health now drive the majority of costs according to the Business Group on Health 2026 Employer Health Care Strategy Survey. Mental health utilization jumped significantly, with 73% of employers reporting increased usage. A meaningful culture of wellness means removing age restrictions on cancer screenings, expanding mental health access through virtual care options, and building advanced primary care models that catch chronic conditions early. The Quantum Health data showing $15.65 saved per member-month from telehealth and urgent care proves that access matters more than traditional wellness lectures.
Centralize Your Health Data to Predict Costly Outcomes
Centralizing health data transforms how you manage costs because fragmented information prevents early intervention. When your claims data, benefits information, and clinical records sit in separate systems, you miss patterns that predict expensive outcomes. Predictive analytics can flag members at risk of costly interventions like surgery, imaging, or opioid use, then guide them into conservative digital physical therapy instead. According to Sword Health’s Predict ROI Report, this approach yields up to a 4.4x return on investment by reducing unnecessary imaging and procedures. The challenge is that relying solely on past high-cost claims misses about 72% of future high-cost members, so you need proactive analytics, not reactive claims analysis. A centralized platform that integrates claims, benefits, and clinical data gives you visibility into patterns that traditional spreadsheets and disconnected systems cannot reveal.
Control Pharmacy Costs Through Strategic Coverage Design
For pharmacy costs specifically, transparency and strategic coverage matter far more than hoping employees choose generics voluntarily. GLP-1 medications now consume significant pharmacy budgets as 79% of employers see increased obesity medication utilization. Rather than absorbing these costs or implementing restrictive prior authorization alone, decouple your coverage from manufacturer rebates, consider biosimilar adoption where available, and implement stricter coverage criteria that tie access to participation in nutrition and diabetes management programs. This approach acknowledges that high-cost medications serve real health needs while preventing them from becoming open-ended expenses that crowd out other essential care. Your pharmacy strategy should reflect the same rigor you apply to medical care-measuring outcomes, holding vendors accountable, and adjusting coverage based on what actually improves employee health.
These foundational strategies set the stage for the next layer: digital health platforms that automate and scale these efforts across your entire workforce.
How Digital Health Platforms Drive Cost Reduction
Real-Time Data Integration Identifies Risk Before Costs Spike
Digital health platforms consolidate claims data, benefits information, and health records into one system where predictive analytics reveal patterns that spreadsheets cannot. The Commonwealth Fund research shows that value-based care models reduce overall costs by emphasizing primary care and cutting unnecessary ER and hospital use, but this only works if your employees access primary care when they need it. A centralized platform solves this problem by integrating multiple data sources to catch risk patterns early, before a member escalates to an expensive procedure.
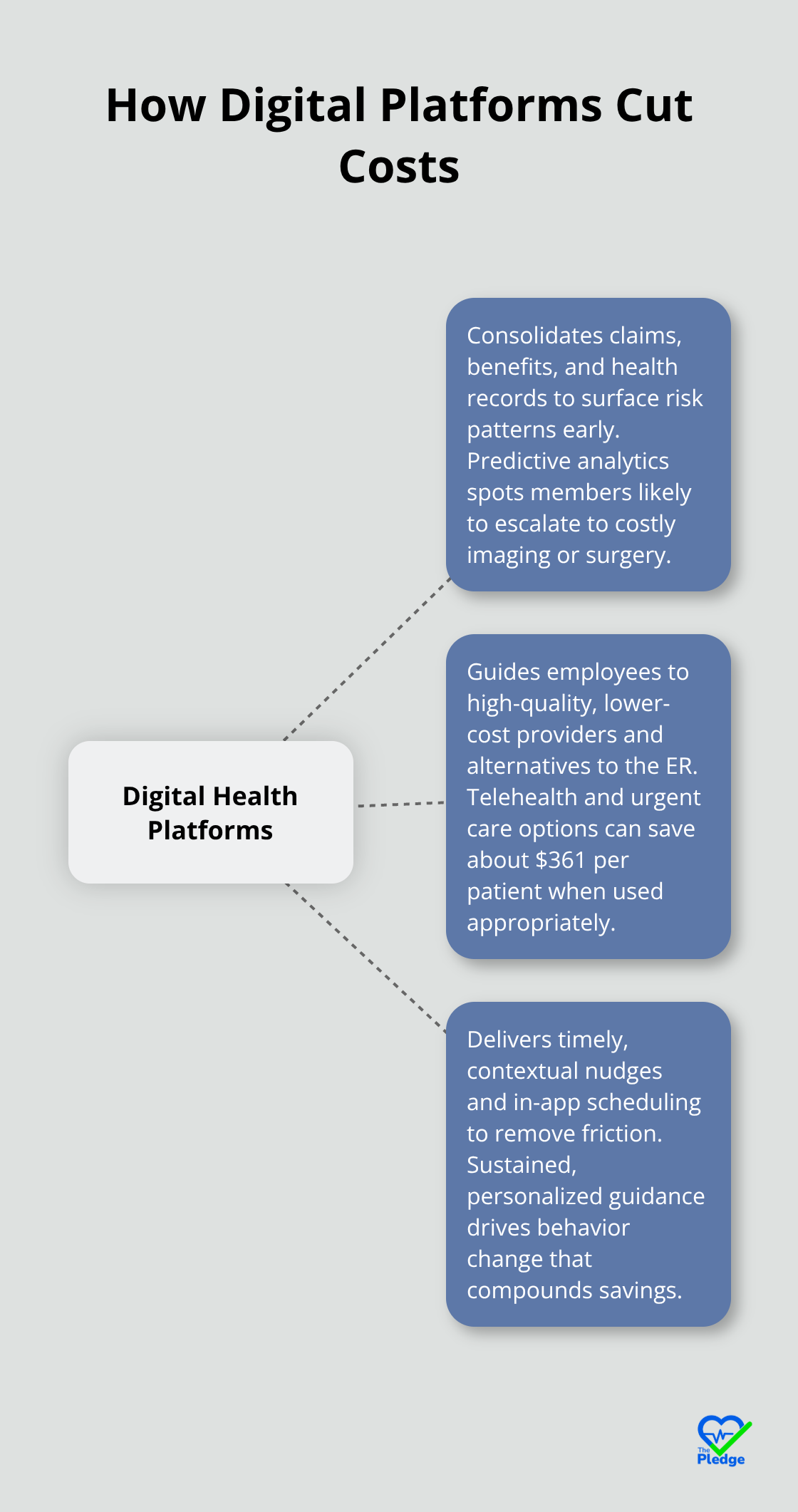
According to Sword Health’s Predict ROI Report, employers using predictive analytics to flag members at risk of costly interventions like surgery or imaging, then steering them toward conservative digital physical therapy instead, achieve up to a 4.4x return on investment. The critical insight is that relying on past high-cost claims catches only about 28% of future high-cost members, meaning reactive approaches leave 72% of expensive outcomes undetected until they happen. Real-time health monitoring and predictive algorithms work together to identify which employees need intervention today, not after they’ve already spent thousands on unnecessary imaging or surgery. This shifts your cost management from reactive claims processing to proactive prevention, which is where actual savings accumulate.
Care Navigation Removes Barriers to Cost-Effective Choices
Care navigation and employee engagement multiply these savings because employees need guidance to use high-quality, cost-effective providers. When employees access a digital platform that shows which providers deliver better outcomes at lower cost, and which urgent care centers cost less than emergency departments for the same condition, they make better decisions. Telehealth and urgent care expansion saves approximately $361 in savings per patient compared with traditional in-home care programs, but only if employees know about these options and can access them easily. A digital health platform removes friction from this process through real-time provider recommendations, appointment scheduling within the platform, and personalized reminders based on each employee’s specific health risks. When your platform sends an employee with diabetes a reminder to schedule their preventive visit, then suggests three nearby primary care doctors with strong outcomes, then lets them book an appointment directly in the app, you’ve eliminated the barriers that usually prevent preventive care.
Personalized Engagement Drives Sustained Behavior Change
Personalized health guidance transforms how employees interact with their benefits. A platform that delivers contextual health information at the moment an employee needs it-rather than generic wellness emails that employees ignore-creates the engagement that actually changes behavior. The combination of predictive analytics identifying who needs care, a centralized platform consolidating all the information, and personalized navigation guiding employees to the right provider at the right time creates the compounding effect that reduces healthcare costs. The platform becomes the operating system for your entire cost management strategy, automating the interventions that would otherwise require manual outreach and coordination across multiple vendors.
Final Thoughts
Reducing healthcare costs in 2025 requires moving beyond reactive cost-cutting and toward systems that catch problems before they become expensive. The strategies outlined here-targeting your actual cost drivers, centralizing health data, and implementing strategic pharmacy coverage-work because they address root causes rather than symptoms. Prescription drugs now consume 27% of your healthcare budget, chronic diseases escalate without early intervention, and emergency department overuse drains resources that preventive care could have avoided.
The financial payoff is real and measurable. Predictive analytics identifying high-risk members before costly interventions occur delivers up to a 4.4x return on investment. Telehealth and urgent care expansion saves approximately $15.65 per member-month by redirecting employees away from expensive emergency departments. Digital-first care pathways for musculoskeletal conditions, one of your largest cost drivers, save around $3,177 per member annually by preventing unnecessary imaging and surgery.
Start with your claims data to identify which conditions consume your budget, then build your preventive care programs, pharmacy strategy, and digital tools around those specific conditions rather than generic wellness activities. A centralized platform like The Pledge integrates your claims data, benefits information, and health records into one system where predictive analytics reveal patterns and personalized navigation guides employees toward high-quality, cost-effective care. The employers reducing healthcare costs most effectively in 2025 aren’t cutting corners on employee health-they’re using smarter systems that align cost reduction with better care.