Most employees spend hours hunting through different portals, emails, and documents just to understand what their health coverage actually includes. At The Pledge, we’ve seen firsthand how fragmented benefits systems drain time and leave people confused about their own healthcare options.
Centralized employee benefits change this entirely. When everything lives in one place, employees find answers faster, use their plans more effectively, and make better health decisions.
Why Benefits Stay Scattered Across Your Organization
Most employers operate with benefits spread across three to five different vendors. HR manages one portal, the insurance carrier runs another, and employees receive wellness program updates through a third channel. This fragmentation isn’t accidental-it’s the result of how benefits evolved. Companies added solutions piecemeal over years, each vendor operating independently without real integration. The result is that employees face a maze of logins, conflicting information, and gaps where critical health data simply disappears between systems.
The Experience Problem Fragmentation Creates
When employees can’t find their coverage details, they don’t use their benefits effectively. Research from the Employee Benefit News webinar on centralized wellness highlighted a major problem: fragmentation creates an experience problem where employees are overwhelmed by multiple portals, leading to low utilization. Most employees spend less than an hour on their plan during the year. This wasted time compounds when someone needs urgent care or faces a health decision. They might not know what their plan covers for a specialist visit, whether they need pre-authorization, or what their actual out-of-pocket cost will be. Worse, they often make healthcare decisions based on incomplete information because finding accurate details takes too much effort.
How Confusion Drives Poor Health Decisions
The stakes are high: employees who don’t understand their coverage delay preventative care, skip screenings, and end up in emergency rooms instead of managing conditions early. This drives up costs for both employers and employees. Insured employees skip care for three main reasons: high out-of-pocket costs, access barriers, and confusion about benefits. When they don’t know about preventative benefits, they miss opportunities to catch health issues early.

When they’re unsure about costs, they avoid care altogether. These decisions ripple through the healthcare system-delayed diagnoses become expensive treatments, preventable conditions become chronic diseases, and emergency care replaces proactive management.
Where Critical Health Information Disappears
When benefits information lives across disconnected systems, critical health signals vanish. A provider updates treatment plans in their system, but that information never reaches the employee’s insurance carrier or their employer’s wellness program. Someone completes a health screening through one vendor, but their doctor never sees those results. Family members who should be informed about coverage can’t access information. These gaps mean duplicate tests, missed preventative opportunities, and fragmented care that costs more and delivers worse outcomes. The employee becomes responsible for manually transferring information between systems-a task most people either forget or get wrong.
What Centralization Solves
Centralized benefits platforms eliminate these disconnects. Instead of hunting across multiple portals, employees access everything from one place. Real-time data flows between employers, insurers, and providers, so critical health information reaches the right people instantly. Employees see their coverage details, understand their options, and make informed decisions faster. This shift from fragmentation to integration transforms how employees engage with their health-and how employers manage costs.
How Centralized Platforms Transform Wellness Access
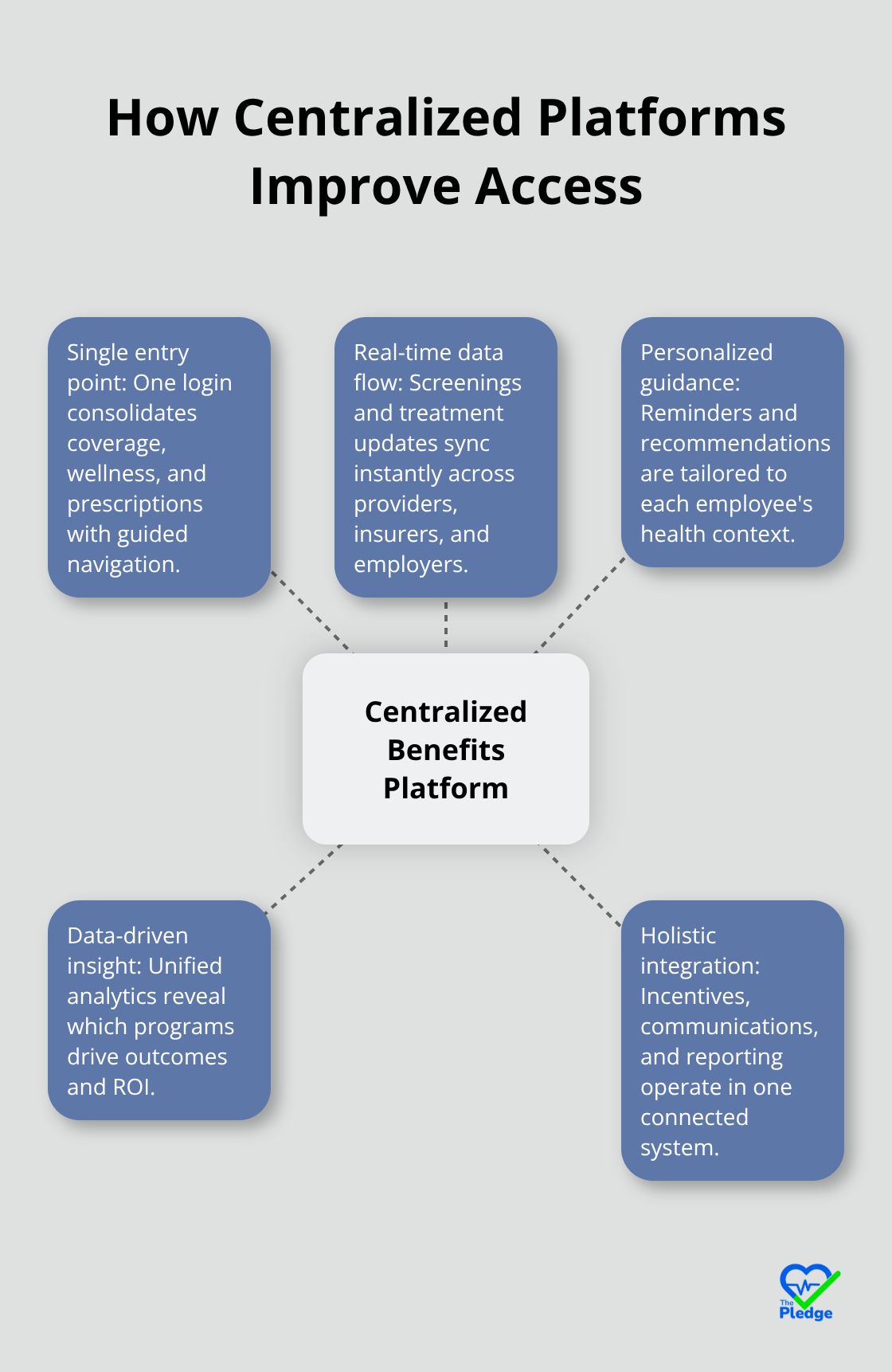
Single Entry Point Eliminates Navigation Chaos
When employees access their benefits through a single platform, everything changes. Instead of logging into separate portals to check coverage, then another to review their wellness program, then a third to understand their prescription benefits, they see it all in one place. A centralized entry point for wellbeing provides guided navigation to the right resources and personalized recommendations, shifting the employee journey from “Where do I go?” to “Here’s where I start.” This simple change transforms how people interact with their health benefits.
Real-Time Data Flow Connects Care Across Systems
The real power emerges when that platform connects to actual health data. When an employee completes a health screening, that information flows directly to their doctor and insurance carrier in real time, not days later through manual processes. When a provider updates a treatment plan, the employee sees it immediately through personalized reminders tailored to their specific health situation. This isn’t about convenience alone-it fundamentally changes how employees engage with prevention.
Research shows that coordinated care in integrated models connects employees to the appropriate level of support, whether clinical care, coaching, or self-guided resources, driving measurable improvements in anxiety, depression, and absenteeism.
Engagement Metrics Prove the Business Case
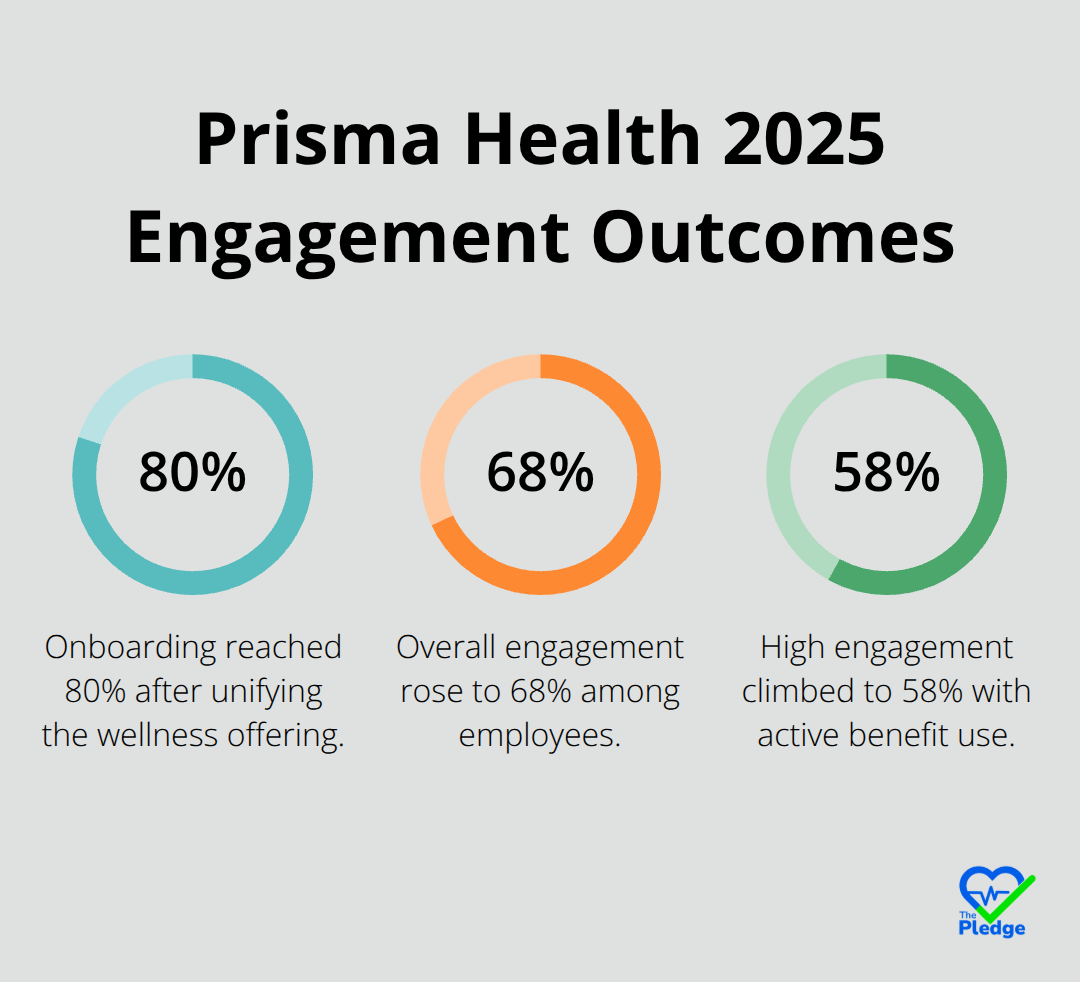
Organizations that implement centralized benefits see engagement climb dramatically. When Prisma Health unified their wellness offering in 2025, onboarding reached 80 percent, engagement hit 68 percent, and high engagement climbed to 58 percent. That same year, they completed over 2,000 additional health screenings because employees actually knew the screenings existed and could access them easily.
The result was that 70.8 percent of participants were categorized as thriving. Data-driven insights from a unified platform provide actionable metrics on engagement, health outcomes, and business impact, allowing HR teams to see exactly which programs drive results and which ones drain resources without delivering value.
Holistic Integration Replaces Fragmented Programs
The workplace wellness market is shifting decisively toward holistic, integrated approaches. Generic wellness programs fail because employees can’t find them, don’t understand how they connect to their benefits, and see them as disconnected from actual healthcare. Successful integration isn’t measured by initial signup spikes-it’s proven through sustained utilization and engagement over time. Employers that consolidate incentive management, communications, and reporting through a single platform reduce administrative complexity while simultaneously improving the employee experience through accessibility, personalization, and human-centered design embedded into one system.
What Happens When Integration Meets Personalization
Personalization at scale uses health survey responses and readiness-to-change levels to tailor pathways, ensuring employees see relevant options instead of generic messaging. Giving employees choice and ownership through guided personalization builds trust and increases engagement. Feedback loops matter only if actions follow; rapid program adjustments in response to input strengthen credibility and trust. This approach scales for large employers with layered vendor ecosystems, transforming how benefits drive actual health outcomes rather than simply checking boxes on compliance requirements. The next step involves understanding how to measure and sustain these improvements over time, which requires the right data infrastructure and commitment from leadership.
Real-World Impact of Centralized Benefits on Health Outcomes
Engagement Metrics That Prove Centralization Works
Centralized benefits platforms produce measurable results that justify the investment. When Prisma Health implemented a unified benefits approach in 2025, their numbers tell a concrete story. Onboarding reached 80 percent, meaning four out of five employees activated their benefits rather than ignoring them. Engagement hit 68 percent, and high engagement climbed to 58 percent, indicating that employees actively used their benefits instead of signing up passively. That same year, they completed over 2,000 additional health screenings because employees knew those screenings existed and could access them without friction. The result was that 70.8 percent of participants were categorized as thriving, a stark contrast to organizations where benefits remain scattered across disconnected systems.
Prevention Catches Conditions Before They Become Expensive
The health impact extends beyond engagement metrics into prevention and cost reduction. According to the CDC, diagnosed diabetes costs $413 billion annually in medical costs and lost productivity, while obesity costs the U.S. healthcare system nearly 173 billion dollars per year. Heart disease and stroke cost 233.3 billion dollars in medical costs and 184.6 billion dollars in lost productivity. These conditions are largely preventable through early screening and lifestyle management, yet fragmented benefits systems make prevention invisible to employees.
When centralized platforms connect employees to preventative care, they catch conditions early when treatment is simpler and cheaper. Coordinated care in integrated models connects employees to the appropriate level of support (clinical care, coaching, or self-guided resources), driving measurable improvements in anxiety, depression, and absenteeism. Employers that consolidate their benefits infrastructure report significant reductions in medical spend because they address root causes and comorbidities earlier, before expensive interventions become necessary.
The Financial Case for Centralization
The cost of implementing a centralized platform recovers quickly through prevented emergency room visits, avoided hospitalizations, and reduced chronic disease management expenses. Employers see the gap between what happens when employees can actually find and use their benefits versus when benefits remain hidden behind multiple portals. Data-driven insights from a unified platform provide actionable metrics on engagement, health outcomes, and business impact, allowing HR teams to see exactly which programs drive results and which ones drain resources without delivering value. Successful integration proves itself through sustained utilization and engagement over time, not initial signup spikes.
Final Thoughts
Fragmented benefits systems waste employee time and hide preventative care opportunities that could transform health outcomes. Centralized employee benefits eliminate this chaos by putting everything employees need in one place, from coverage details to health screenings to personalized reminders that prompt action. Organizations that consolidate their benefits infrastructure see engagement climb to 68 percent, onboarding reach 80 percent, and measurable improvements in health outcomes that directly reduce costs.
Technology makes this transformation possible, but only when it’s designed around the employee experience. The right platform connects all the pieces without adding complexity, personalizes guidance based on individual health needs, and sends reminders that matter rather than clutter inboxes. When employees access their benefits through a single system with real-time data flowing between providers, insurers, and employers, they make better health decisions and complete preventative screenings that catch conditions early.
The Pledge centralizes health data, integrates with existing benefits, and uses AI-driven technology to coordinate care across your entire health ecosystem. Our platform achieves 4x industry-standard engagement rates because it removes friction and puts employees in control of their health journey. Start by auditing your current vendor ecosystem and identifying where critical health information gets lost, then move toward integration.