Patients today face a maze of disconnected providers, insurance details, and medical records scattered across multiple systems. This fragmentation leads to missed appointments, duplicate tests, and costly mistakes that could have been prevented.
Care navigation tools are changing this reality by bringing everything together in one place. At The Pledge, we’ve seen firsthand how the right platform empowers patients to take control of their healthcare journey.
Why Patients Struggle to Navigate Healthcare
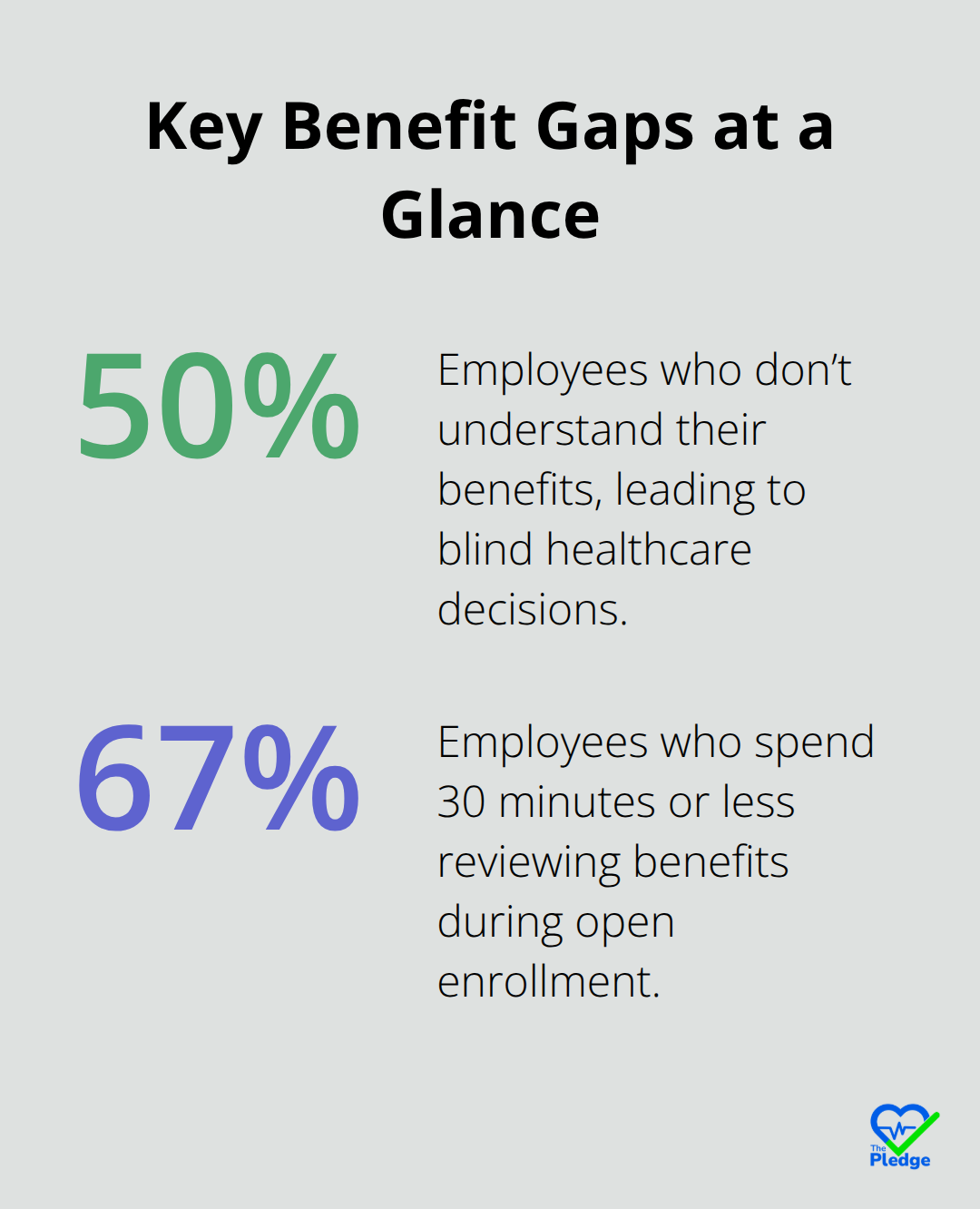
Healthcare systems in 2026 remain fundamentally broken when it comes to patient experience. A patient with a chronic condition has their primary care records at one clinic, specialist notes scattered across three different hospital systems, pharmacy data locked in another database, and insurance information buried in yet another portal. None of these systems talk to each other. When a patient needs to schedule an appointment, they often have no idea what their insurance will cover, whether they’ll face a surprise bill, or if their chosen provider is even in-network. Guardian Life Insurance found that 50% of employees don’t understand their benefits, which means half your workforce makes healthcare decisions blind. This fragmentation isn’t a minor inconvenience-it directly causes medical errors.
A patient might undergo duplicate testing because their previous results aren’t accessible to their current provider. Another might skip a necessary follow-up because they forgot the appointment date or didn’t receive a reminder. The consequences compound quickly: missed preventive care leads to more emergency room visits, which cost employers and individuals far more than coordinated care would have.
Information Overload Paralyzes Decision-Making
Beyond fragmentation sits another barrier: sheer information overload. During open enrollment, 67% of employees spend 30 minutes or less reviewing their benefits, according to Voya Financial. In that compressed window, they must understand deductibles, copays, out-of-pocket maximums, network restrictions, and coverage exclusions across medical and pharmacy benefits. Most people fail this test. When a patient finally decides to seek care, they face more decisions: which provider should they see, how much will it cost, and should they go to urgent care or the emergency room? Without upfront cost transparency, patients avoid care altogether or end up in the most expensive setting by default. Team-based care navigation shows the strongest signal for improving appropriate service use, according to research in BMC Health Services Research 2023. Yet most patients navigate alone, armed only with vague assumptions about their coverage and no clear way to compare providers by quality, cost, or availability. The result is decision paralysis or, worse, decisions made on incomplete information that lead to unnecessary procedures, wasted money, and poor health outcomes.
Why Care Navigation Tools Matter Now
The gap between what patients need and what healthcare systems provide has never been wider. Patients require a single entry point that consolidates their medical records, benefits eligibility, provider options, and cost estimates in real time. They need clinical guidance from qualified professionals (nurse practitioners, RNs, licensed social workers) who understand their medical history and preferences. They need appointment scheduling that considers their location, insurance status, and availability. Most importantly, they need transparency about what care will cost before they commit to it. Without these elements, patients remain trapped in a fragmented system that rewards complexity and punishes those who can’t navigate it alone. The next section explores how modern care navigation platforms address each of these gaps and what employers and health plans can expect from a truly integrated solution.
How Care Navigation Platforms Transform Healthcare Access
Modern care navigation platforms eliminate the fragmentation that defines patient frustration. Instead of juggling multiple portals, phone calls, and paper records, patients access a single interface that aggregates their medical history, insurance coverage, provider networks, and real-time pricing data. When a patient logs in, they see their upcoming appointments, medication refills, preventive care reminders, and available providers matched to their specific plan and location. This consolidation matters because it transforms decision-making from a guessing game into an informed process. A patient no longer wonders whether their chosen specialist is in-network or calls their insurance company to verify coverage; the platform displays this information instantly alongside out-of-pocket cost estimates.
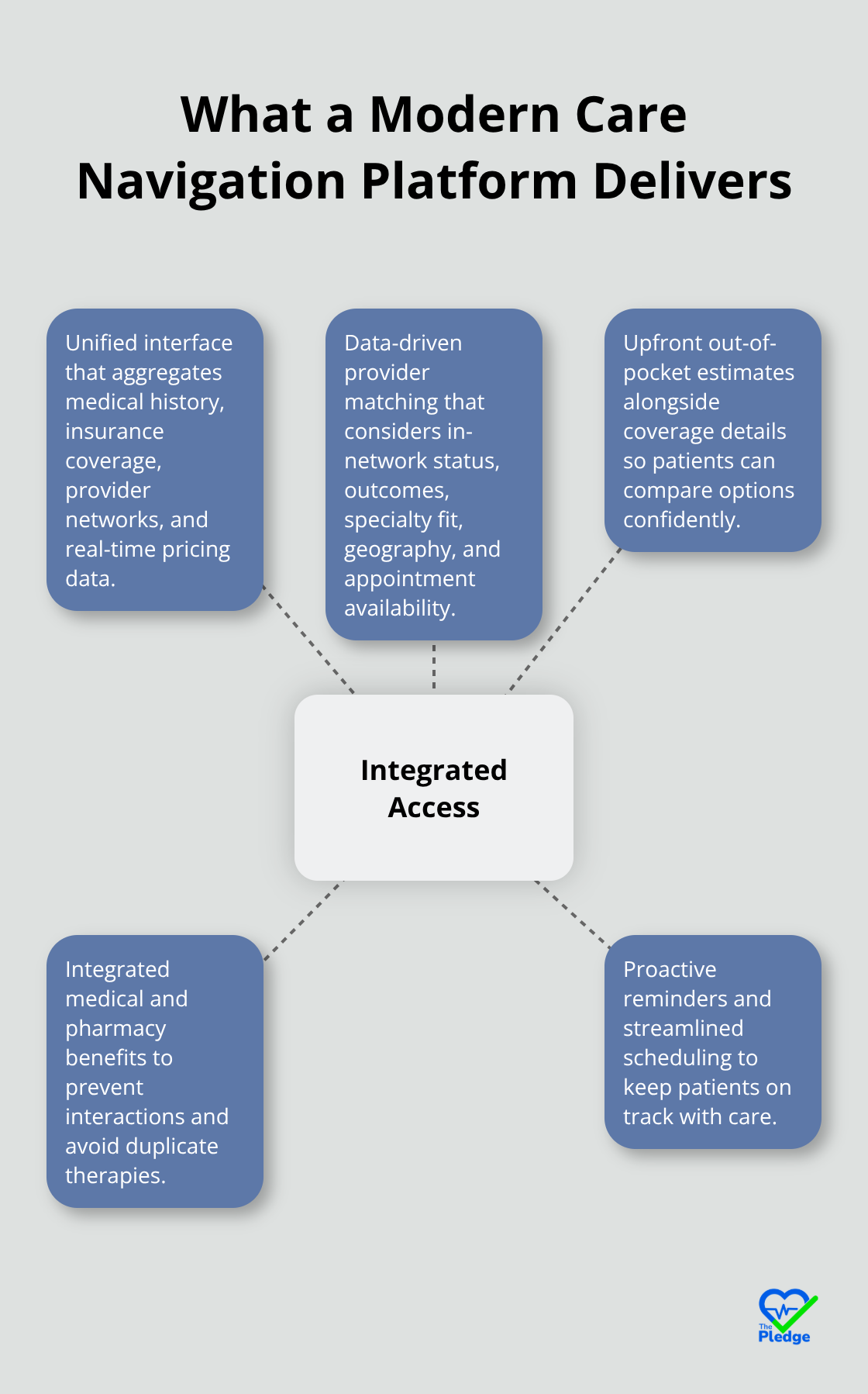
Team-based care navigation produces measurably better outcomes in appropriate service utilization compared to traditional fragmented care. The platform’s integration of medical and pharmacy benefits creates a unified view that prevents costly medication interactions and duplicate therapies across providers who otherwise would never communicate.
Real-Time Scheduling Removes Administrative Friction
Appointment scheduling through traditional channels wastes enormous amounts of time. Patients call provider offices, wait on hold, receive a date weeks away, and then forget the appointment because no reminder arrives. Care navigation platforms automate this entirely. Intelligent scheduling engines identify high-quality, in-network providers with available appointments and book visits across multiple modalities: same-day video consultations, in-person visits, and 24/7 chat-based urgent care. The platform sends appointment confirmations, pre-visit intake forms, and multiple reminders at strategic intervals. This reduces no-show rates and ensures patients arrive prepared with necessary medical history already uploaded. For complex cases, the system coordinates across specialists, managing referrals and follow-ups that typically fall through cracks in fragmented systems. Patients spend less time on administrative tasks and more time on actual care. Employers see reduced HR burden because employees no longer flood benefits departments with questions about provider availability or coverage eligibility.
Provider Matching Guided by Quality and Cost Data
Selecting the right provider requires information most patients lack: quality metrics, patient satisfaction scores, cost comparisons, and specialist availability. Care navigation platforms aggregate this data and match patients to providers based on multiple criteria simultaneously. The matching algorithm considers in-network status, specialty expertise, geographic location, appointment availability, and documented patient outcomes. When a patient needs orthopedic surgery, for example, the platform surfaces surgeons who specialize in their specific procedure, displays their complication rates relative to peers, shows negotiated costs for that exact surgery, and indicates wait times. This transparency fundamentally changes patient behavior. Instead of defaulting to the nearest provider or whoever their doctor suggests, patients make deliberate choices informed by quality and cost. The platform’s data-driven approach reduces unwarranted variation across settings and medications, improving outcomes while controlling costs. For employers, this steering effect translates directly to lower total healthcare spend because members route to preferred, high-value providers with negotiated pricing rather than expensive out-of-network alternatives.
Upfront Cost Transparency Prevents Surprise Bills
Patients avoid care when they fear unexpected costs. Care navigation platforms eliminate this barrier through upfront price estimates that show exactly what a patient will pay before they commit to treatment. The system displays deductibles, copays, out-of-pocket maximums, and total cost of care in plain language. When a patient compares two providers for the same procedure, they see the actual price difference and understand how their insurance plan affects their final bill. This visibility enables more deliberate decisions and helps members manage their healthcare spending strategically. Patients no longer face surprise bills because they understand their financial responsibility in advance. Employers benefit from this transparency because engaged employees make cost-conscious choices that reduce overall plan spend. The combination of price visibility and provider quality data creates a powerful incentive structure: patients naturally gravitate toward high-value care when they can see both the quality metrics and the cost implications side by side.
Measuring Real-World Healthcare Impact
Care navigation platforms deliver measurable results because they address the root causes of healthcare waste. When patients access consolidated medical records, transparent pricing, and guided provider selection, their behavior shifts immediately. They schedule appointments earlier, choose high-value providers over expensive alternatives, and avoid unnecessary emergency room visits. Real-world implementations prove this effect consistently across diverse patient populations and healthcare settings.
Team-Based Navigation Improves Service Utilization
A systematic review of primary care-based navigation studies examined participants and found that team-based navigation models produced improvements in appropriate service utilization. These weren’t theoretical gains; they represented actual shifts in where and how patients sought care. In the Health TAPESTRY trial conducted in Canada, older adults connected to community supports through navigation showed fewer hospitalizations compared to those receiving usual care. The Queensland nurse navigator program deployed 400 navigators by 2019 targeting high-need chronic disease patients and documented reduced readmissions with potential cost savings that continued through ongoing evaluation. These programs worked because navigators removed barriers to appropriate care, preventing patients from defaulting to expensive emergency settings when lower-cost alternatives existed.
Transparent Pricing Steers Patients Toward High-Value Care
Upfront cost transparency steers members toward in-network, high-quality providers with negotiated rates, which reduces total healthcare spend across medical and pharmacy benefits. When patients understand the price difference between a $500 urgent care visit and a $3,000 emergency room visit for the same condition, they make deliberate choices that align with both their financial interests and the employer’s bottom line. Reduced duplicate testing, fewer unnecessary procedures, and lower emergency utilization compound these savings over time. For individuals, care navigation eliminates surprise bills and prevents the costly consequences of delayed care.

A patient who schedules a preventive visit through the platform avoids the expensive downstream complications that emerge when conditions go unmanaged.
Medication Adherence Reduces Hospital Readmissions
Care navigation platforms improve medication adherence through reminders and coordinated pharmacy benefits, which prevents hospital readmissions driven by patients missing doses. When patients receive timely notifications about refills and understand their medication regimen within the context of their overall care plan, they maintain treatment consistency. This adherence translates to fewer acute episodes and reduced emergency utilization. The integration of medical and pharmacy data surfaces potential drug interactions before they cause harm, further protecting patient safety and reducing costly complications.
Investment in Navigation Infrastructure Generates Returns
Germany’s Innovationsfonds invested approximately 200 million euros annually through 2024 in navigator programs, recognizing that the upfront cost of structured navigation infrastructure generates substantial returns through reduced acute utilization and improved chronic disease management. This large-scale commitment reflects a fundamental shift in how healthcare systems view navigation-not as an optional service but as essential infrastructure that reduces total cost of care. Employers who implement care navigation platforms see measurable improvements in plan performance, employee satisfaction, and healthcare spending trends that compound over multiple years.
Final Thoughts
Care navigation tools address a fundamental problem that healthcare systems have failed to solve: patients lack a single, trustworthy place to manage their health. The fragmentation, information overload, and cost uncertainty that plague healthcare today aren’t inevitable-they result from systems designed around provider convenience rather than patient needs. Modern platforms eliminate these barriers by consolidating medical records, benefits data, provider options, and pricing information into one interface where patients make informed decisions.
The evidence proves that team-based navigation improves appropriate service utilization, transparent pricing steers patients toward high-value care, and real-time appointment scheduling removes administrative friction. Germany’s sustained investment of 200 million euros annually in navigator programs reflects a recognition that care navigation infrastructure generates measurable returns through reduced acute utilization and improved chronic disease management. Employers and health plans respond to this evidence because the financial case remains undeniable: lower total healthcare spend, higher employee engagement, and reduced HR burden.
We at The Pledge built a platform that embodies these principles through AI-driven systems that centralize health data and coordinate care across all stakeholders. Explore The Pledge to see how care navigation transforms both employee health and your bottom line.










