Your family’s health information is scattered across different doctors, hospitals, and clinics. Nobody has the full picture-not even you.
At The Pledge, we believe care coordination across families shouldn’t require a spreadsheet and a phone tree. When family members can access shared health records, coordinate appointments, and alert each other to important changes, everyone stays healthier.
Why Your Family’s Medical Records Are Trapped in Different Systems
Healthcare fragmentation isn’t a minor inconvenience-it’s a systemic failure that directly harms families. According to a National Institutes of Health survey, the United States has the highest share of poor care coordination among 11 high-income countries studied, at 9.8% of the population experiencing fragmented care. This fragmentation creates real consequences. When your mother’s cardiologist doesn’t know about her diabetes medication, when your child’s school nurse can’t access allergy information, or when duplicate lab work happens because test results never reach the right doctor, families pay the price in both health outcomes and money. The average family member manages appointments, medications, and medical histories across at least three separate healthcare systems, often without any central way to share information. Nobody has the complete picture-not the patient, not the family, and certainly not the providers who need it most.
The Cost of Siloed Information
Duplicated tests represent a staggering waste. When providers can’t access existing lab results or imaging studies, they order them again. A systematic review of cross-sector care coordination programs found that 42% of programs lacked meaningful information sharing across providers, creating exactly this scenario.
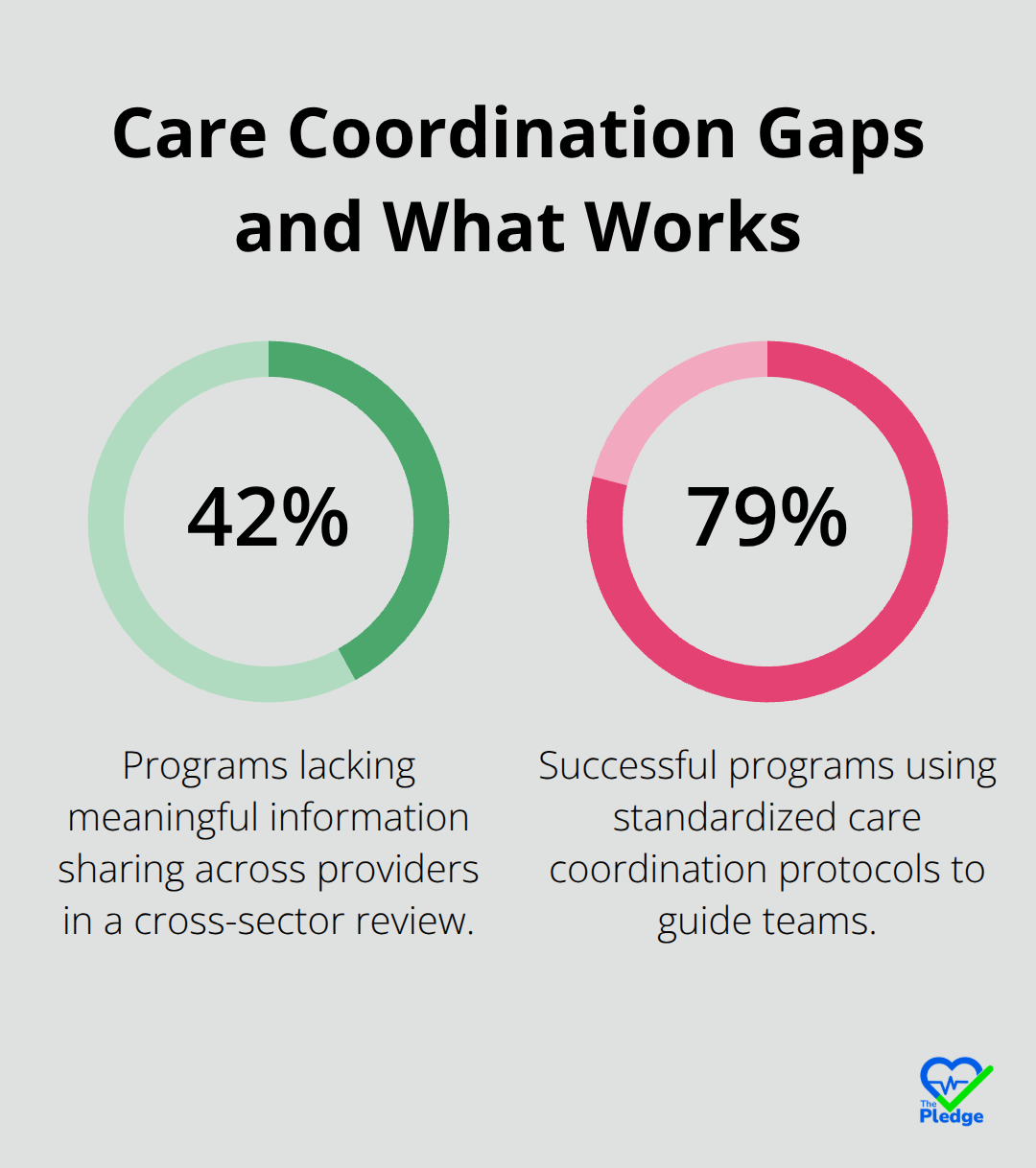
For families managing chronic conditions or complex medical needs, this redundancy adds up fast-both in medical bills and in patient frustration. Communication gaps between providers lead to conflicting treatment plans. One doctor increases a medication while another decreases it. Preventative care opportunities get missed because nobody coordinates follow-up care after a hospital discharge. Studies show that effective discharge planning and post-discharge follow-up directly reduce hospital readmissions, yet most families navigate this transition alone, piecing together information from discharge papers and phone calls.
Why Active Referrals Matter More Than You Think
Passive referrals-where a doctor simply tells you to see a specialist-fail families constantly. Research found that active referrals where staff help patients schedule appointments improve care coordination outcomes. This distinction matters enormously. When families receive a referral without active support, enrollment in recommended services drops significantly. Among families referred to needed services, only 53.8% were actually enrolled within 4–6 months. For families already managing complex medical situations, the burden of making calls, waiting on hold, and navigating insurance approvals becomes the barrier that prevents care from happening at all. Active engagement-real people helping families navigate the system-changes outcomes.
What Unified Platforms Can Accomplish
Centralized health information transforms how families coordinate care. When all family members access shared medical records, real-time alerts for appointments and medications reach everyone who needs them. Providers gain visibility into the complete medical picture, which eliminates redundant testing and prevents conflicting treatment plans. Families no longer piece together information from multiple sources or repeat their medical history to each new provider. This shift toward unified platforms addresses the core problem: information trapped across disconnected systems. The next section explores how these platforms actually work in practice and what features matter most for your family’s health.
What Unified Platforms Actually Do for Your Family
Unified health platforms eliminate the administrative burden families face when coordinating care across multiple providers. Rather than calling three different offices to confirm your child’s allergy information or manually tracking which medications your aging parent takes, a centralized platform makes this information instantly accessible to everyone who needs it. The core function is straightforward: one secure location where family members, providers, and insurers access the same medical records, medication lists, and appointment schedules simultaneously. This eliminates the scenario where your daughter’s pediatrician doesn’t know she received treatment for an ear infection at an urgent care clinic last week, or where your spouse’s cardiologist prescribes something that conflicts with medication your primary care doctor recommended. When 42% of care coordination programs still struggle with basic information sharing across providers, a unified platform becomes the infrastructure that makes coordination actually possible instead of aspirational.
Real-Time Coordination Prevents Medical Errors
The moment a provider updates your medical record, family members designated on your care team receive alerts. If your mother’s dosage changes or a new diagnosis appears in the system, you know immediately. This speed matters enormously for medication safety.
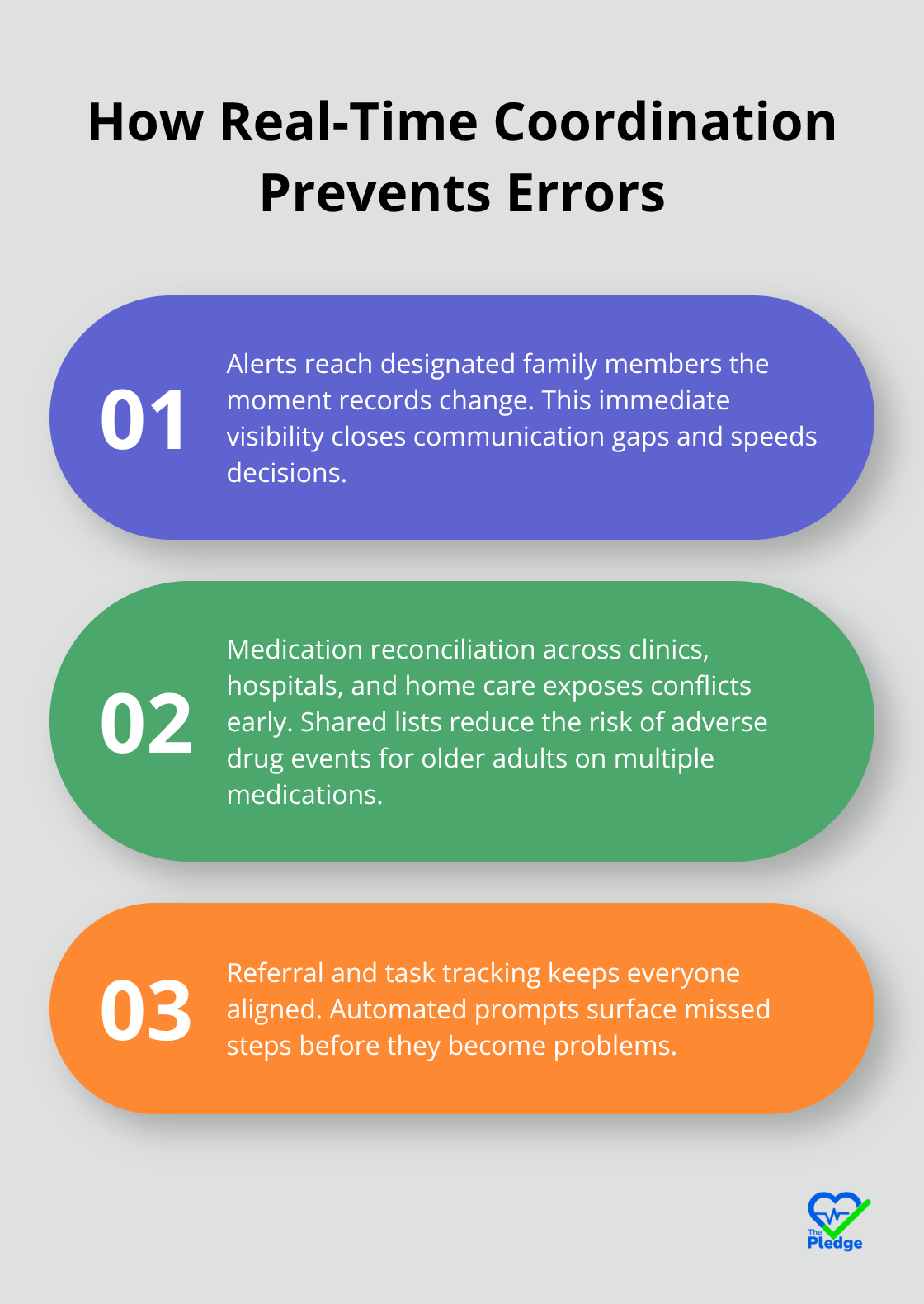
Research shows that medication reconciliation across hospitals, clinics, and home care significantly reduces adverse drug events, particularly for older adults managing multiple medications. A unified platform automates what families currently do manually: tracking which provider prescribed what, when refills are due, and whether new medications interact with existing ones. When your father fills a prescription at one pharmacy and your mother uses another, neither pharmacist has visibility into his complete medication list. A unified platform integrates pharmacy data so that potential interactions surface before medication reaches the patient. Active engagement from staff also improves outcomes substantially. Studies found that when coordinators actively help families enroll in needed services, rather than simply providing a referral, enrollment rates jump dramatically. A unified platform enables this through automated reminders, referral status tracking, and alerts that notify coordinators when families need follow-up support.
Coordinated Care Planning Reduces Hospital Readmissions
Effective discharge planning directly reduces readmissions, yet most families receive a stack of papers at hospital discharge with no coordinated follow-up. A unified platform creates a documented care plan that all providers access. Instead of your mother wondering whether she should see her cardiologist before or after her physical therapy appointment, or whether her diet restrictions from the hospital apply long-term, the care plan specifies exactly what happens next. Standardized protocols embedded in these platforms guide the entire care team. Research examining cross-sector care coordination found that 79% of successful programs used standardized care coordination protocols that specify enrollment processes, care pathways, and team communication. This removes guesswork. When your child transitions from pediatric to adult care, a unified platform transfers the complete medical narrative so the adult provider understands developmental history and established treatment patterns. The alternative-starting from scratch with a new provider who has no context-creates gaps where care falls apart. Families managing children with complex needs spend enormous time explaining the same history repeatedly. A systematic review found that care coordination for families with neurodevelopmental diagnoses focused heavily on education and family engagement, comprising roughly half of all coordination efforts. A unified platform reduces this burden through accessible information, so families spend less time repeating themselves and more time focused on actual health management.
What Happens When Families Take Control
Families gain visibility into their complete health picture when information lives in one place. Appointment reminders reach everyone simultaneously. Medication lists update in real time across all family members’ devices. Providers see the full context of a patient’s care history instead of isolated snapshots. This shift transforms how families prevent problems before they escalate into emergencies or hospitalizations. The next section explores how these platforms actually integrate with your existing healthcare providers and what features matter most when selecting a solution for your family.
What Unified Care Actually Changes
Healthcare fragmentation costs money in ways families rarely see until the bill arrives. When providers operate in silos, families experience the consequences through redundant tests, missed preventative care opportunities, and preventable hospital readmissions. A systematic review of cross-sector care coordination programs found that frequent patient contact reduced hospitalizations in participating programs. This matters enormously because hospital readmissions represent one of the largest preventable costs in healthcare.
How Structured Discharge Planning Prevents Readmissions
Discharge planning becomes structured rather than chaotic when families coordinate care through unified platforms. Instead of your mother leaving the hospital with vague instructions and hoping she remembers what the discharge nurse said, a coordinated care plan specifies exactly which appointments happen first, which medications change, and who monitors recovery. This specificity prevents the scenario where she misses a critical follow-up appointment or takes conflicting medications because nobody coordinated the transition. Research shows that effective discharge planning directly reduces readmissions, yet most families navigate this alone. Unified platforms eliminate that gap by creating documented accountability across the entire care team.
The Productivity Impact on Employees and Families
The productivity impact extends beyond individual health outcomes. When employees spend three hours weekly managing fragmented medical information for aging parents or children with chronic conditions, that time comes directly from work. Employers report measurable productivity gains when families access coordinated care efficiently because employees focus on jobs rather than navigating healthcare systems. For families managing neurodevelopmental diagnoses, care coordination consumed nearly nine hours over four to six months, with roughly half that time devoted to family education and engagement. A unified health view compresses this timeline dramatically by centralizing information that families currently gather through repeated phone calls and provider visits.
Connecting Families to Healthcare Financing Programs
Healthcare financing represents another significant barrier that coordination addresses. Children accessing structured care coordination programs were successfully enrolled in healthcare financing programs, yet families without coordination often miss these resources entirely because nobody connects them. Active referrals-where staff help families actually enroll in services rather than simply providing a name and number-show enrollment rates of 53.8% within four to six months. This distinction reveals a hard truth: referral information alone fails families. They need people actively guiding them through enrollment processes.
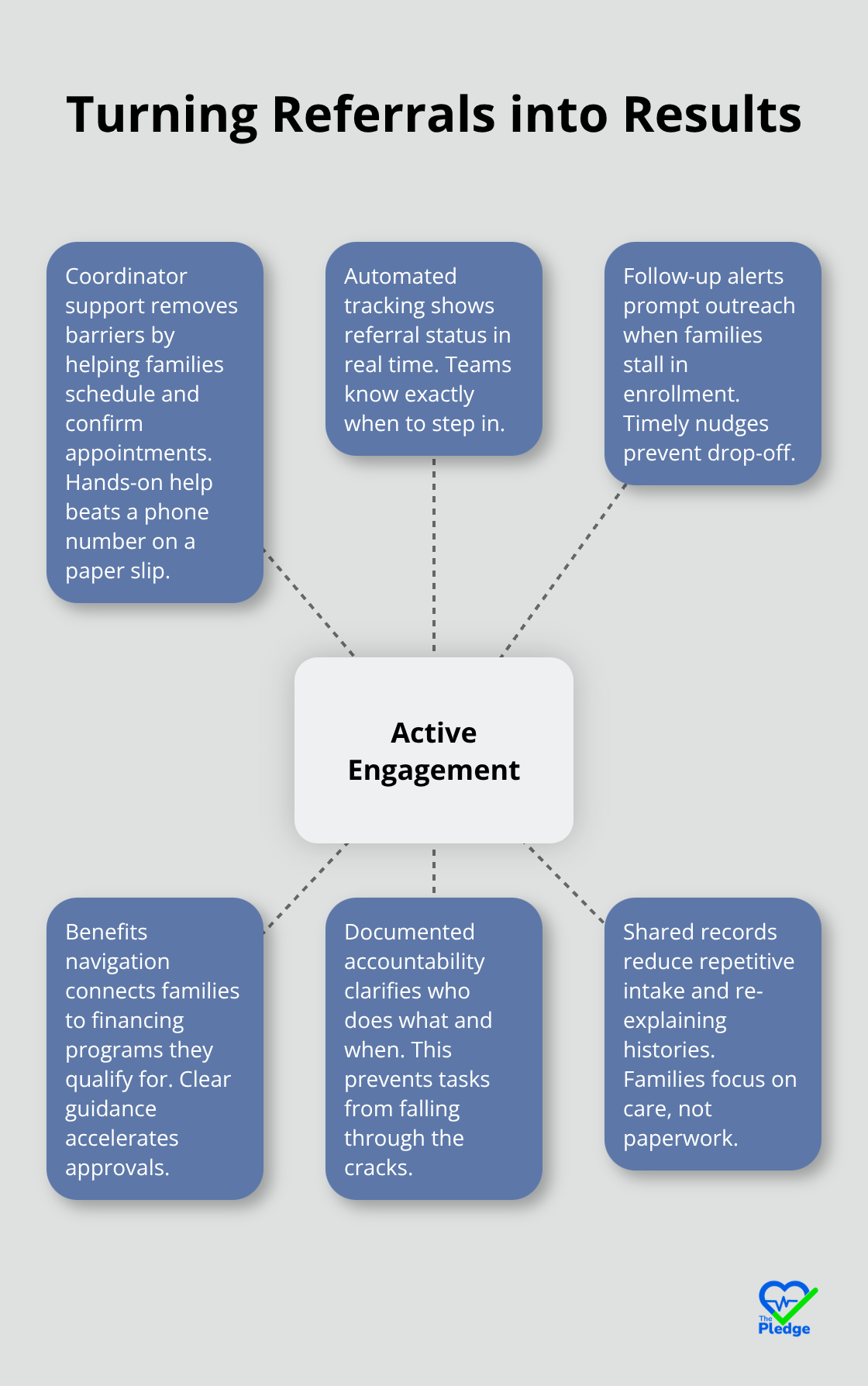
Unified platforms enable this through automated tracking that alerts coordinators when families need follow-up support, transforming passive referrals into active engagement that actually results in families accessing needed services.
Final Thoughts
Care coordination across families works because it addresses the actual problem: information scattered across disconnected systems. Structured care coordination reduces hospitalizations, active engagement increases service enrollment, and standardized protocols eliminate conflicting treatment plans. These documented outcomes from programs already operating across the country prove that unified health platforms transform fragmented chaos into coordinated action.
Technology enables this transformation by centralizing data that currently lives in separate offices, hospitals, and clinics. Real-time alerts reach family members simultaneously, medication lists update across all devices, and providers see complete medical context instead of isolated snapshots. This visibility prevents the gaps where care falls apart and families suffer consequences in both health outcomes and costs.
At The Pledge, we help families coordinate care across multiple providers through unified health platforms that centralize vital medical information and facilitate secure data sharing. Healthcare delivery continues to shift toward family-centered models because fragmentation costs too much in money, time, and preventable health crises. Unified platforms have become the standard infrastructure that makes coordinated care actually possible.










